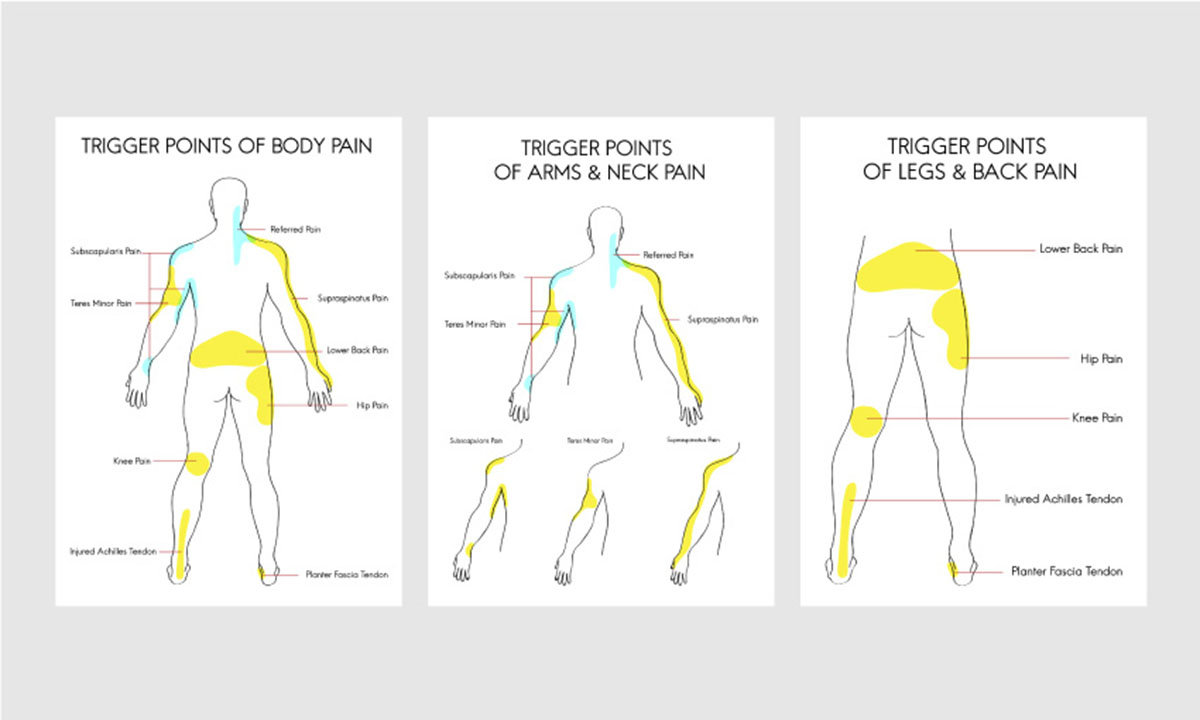
Tender points are one of the defining features of the chronic functional pain disorder fibromyalgia. So-called "trigger points" — a common characteristic of chronic myofascial pain — are different in that they lead to pain that radiates outward from the source, a phenomenon known as "referred pain". Because many fibromyalgia patients also experience myofascial pain, it is not surprising that tender points and trigger points are sometimes confused.
Symptoms of Fibromyalgia
Fibromyalgia can produce a rather broad range of symptoms that are unique in every patient and will also periodically get better or worse. Seasonal changes, your levels of physical activity, and how stressed you are all represent factors that impact the severity of your symptoms at any given time. Fibromyalgia sufferers can, however, expect to be plagued by some combination of widespread pain, fatigue, sensory sensitivity, sleeping difficulties, stiffness, headaches, irritable bowel syndrome, and so-called "fibro fog" — cognitive challenges associated with the disorder. Let's take a closer look at these.
Widespread pain
"Widespread pain" is both pretty descriptive and actually rather vague — you may experience discomfort or downright agony all over your body, or your pain may be concentrated in localized areas, often the back and neck. Though the pain may lift slightly during some periods, you're probably going have some level of discomfort more or less constantly.
Fibromyalgia-related pain may present itself in the form of:
- Sharp, stabbing sensations
- Dull aches
- Burning feelings
Sensitivity to any kind of touch
It's not normal to scream out in pain when someone gives you a pat on the shoulder — but if you have fibromyalgia, it may just happen. Overactive nerves make people with fibromyalgia incredibly sensitive to pain input, and if even that pat on the shoulder hurts, bumping into a table or dropping something on your foot is going to be excruciating. The sensitivity likely won't be limited to physical stimuli, either. Loud noises, bright lights, smells, foods, and smoke can all send you into sensory overload.
Stiffness
Feeling stiff is another common fibromyalgia symptom, which may be at its worst when you've just woken up or done desk work for hours — that is, maintaining the same position for a good while increases your stiffness. Painful muscle spasms are likewise associated with this stiffness.
Fatigue and poor sleep quality (frequent waking, an inability to sleep, or non-restorative sleep)
Getting a good night's sleep is a challenge when you suffer from chronic pain, and fibromyalgia patients often find they wake up several times a night, just can't sleep, or wake up feeling like they haven't slept at all, even if they actually got more than their obligatory eight hours in.
Poor sleep quality is one of the reasons folks with "fibro" suffer from fatigue. Your fatigue levels may range from a mild, low-level "sleepy head" feeling — the type of tiredness most people experience after not getting enough sleep — to an all-out "I really can't function today" situation.
Fibro fog
When you hear that people with fibromyalgia frequently suffer from "cognitive problems" aka fibro fog, you may feel a little insulted, thinking that your intelligence is under attack. Keep in mind, however, that long-term extreme fatigue alone will induce the very same cognitive — "relating to thinking" — difficulties people with fibro deal with. These symptoms are collectively known as fibro fog, and as the term suggests, they cloud your thinking. You may:
- Suffer from short-term memory problems — new information doesn't stick, and you may forget appointments or lose track of where you left things
- Find it very hard to concentrate on everyday tasks
- Have slow or confused speech, and find it tricky to keep up with conversations
Headaches
Headaches, especially migraines but also milder headaches, are another often-seen symptom in people suffering from fibromyalgia. Those patients who struggle with neck and shoulder stiffness are especially likely to be affected. Note that migraine often induces nausea as well.
Irritable bowel syndrome (IBS)
Irritable bowel syndrome, a digestive-system disorder, isn't uncommon in people with fibromyalgia. Stomach pain or cramps, which can be severe, are a common symptom, along with abdominal bloating and alternating constipation and diarrhea.
Depression
It is only logical that a condition that leaves you in constant pain, feeling tired and unable to function can make you depressed in the long run. In addition, fibromyalgia may cause hormonal imbalances that make depression and anxiety even more likely.
Fibromyalgia treatment
Some experimentation may be necessary before you land on a treatment plan that works well for you, so your healthcare provider(s) will be an invaluable partner in the process. Some people with fibro may see a number of specialists; neurologists, gastroenterologists, psychologists and rheumatologists are all sometimes involved in the treatment of fibromyalgia.
Myofascial Pain Syndrome Symptoms
Another chronic pain disorder that may strike people already suffering from fibromyalgia, myofascial pain syndrome causes referred pain following pressure on trigger points, which are especially sensitive spots within your muscles. Because the pain doesn't necessarily manifest anywhere near its origin point, you may have no idea where the pain comes from. Myofascial pain syndrome often sets in after a person makes the same kinds of motions over and over again for a long period of time — this may happen over the course of your professional life, but also after a muscle keeps contracting on its own.
The following symptoms can alert you that it's time to look into myofascial pain syndrome more closely:
- Pain — both chronic and increasing, and which may be so bad that you can't sleep
- Severe muscle aches
- Sore "knots" within a muscle or multiple muscles
Treatment options for Myofascial Pain Syndrome
Non-pharmacological treatment can be extremely helpful, so we'll take a look at options your doctor may suggest.
- Stretching therapy is done under the care of a physical therapist, who will teach you how you can find relief from the pain originating in specific muscles. When trigger points get in the way, numbing medications can help you get through.
- Posture training. Proper posture is very important for everyone, but can particularly help people with myofascial pain syndrome find relief. Posture training is more complex than it sounds, as exercises that target particular muscles can help prevent you from reverting to a harmful posture you may have grown used to over time.
- Massage. Massage, again performed by a physical therapist, can target trigger points, relieving tension and pain. When suffering from both fibromyalgia and myofascial pain chiropractic care might also be beneficial.
- Heat, whether from hot packs or showers, can also ease some of your discomfort.
- Injections sometimes play an important role in the path to symptom relief too. Your healthcare provider may inject a numbing solution or steroid into a trigger point, but sometimes just inserting a needle is enough to relieve tension. This process is known as "dry needling", and your doctor will target areas around the trigger point itself. Acupuncture, administered by a qualified professional, is another option.
- Ultrasound therapy relies on sound waves. It can help heal muscles and relieve pain by promoting a good circulation and offering warmth.
- www.ncbi.nlm.nih.gov/pubmed/7595112
- www.ncbi.nlm.nih.gov/pmc/articles/PMC3258006/
- Walter Frontera Julie Silver Thomas Rizzo: Essentials of Physical Medicine and Rehabilitation 3rd Edition Musculoskeletal Disorders, Pain, and Rehabilitation
- www.ncbi.nlm.nih.gov/pubmed/11871683
- Photo courtesy of SteadyHealth.com


Your thoughts on this