It is well known amongst the medical community (specifically since 1990) that Opioid pain medication can cause the sphincter of Oddi to become un-responsive, or under-responsive.
The Oddi is what opens and closes to let the bile enter the duodenum (small intestine traversing just below the stomach).
(BELOW, at end is a short but comprehensive explanation of the Hepatic system with Gallbladder and functions)
Persons who have Gallbladder (from here on will be noted as GB) issues AND are taking opioid pain medication (i.e. any morphine based/derived product-- percocet, dilaudid, vicodin, morphine, etc... any drug derived from the poppy plant (known as an opiate, e.g. opioid (meaning opiate-like)) may not need surgery.
Here lies the reason:
Opioids cause a number of bodily effects, from pain relief to elongating the intestine (hence causing constipation) to making the GB and its parts react slowly or lazily.
In tests done persons having had HIDA scans done (in real time) were injected with Naloxone (Narcan, an 'anti-opioid') had thier GB's and the Oddi go from little to no function-- to fully functional within a span of several minutes or less.
The patient had GB problems, and took opioid pain medication as well. When the opioid effect was removed the GB function was restored fully, or nearly so.
There is, and can be, a viscious cycle with regards to this.
For example, a person takes pain medicine for one reason, the medicine can cause GB issues, which causes pain. The patient takes more medication for the pain, causing the GB issues to worsen, and so on.
Conversely, a person with GB issues who starts taking opioid pain medication can mask the pain for a while, thus allowing it to go undiagnosed for a span of time until it becomes too pernicious to avoid, therefore needing surgery because a rupture from distention of the GB and biliary duct (either with calculi (gall-stones: made of calcium, magnesium, sodiums, etc)) from having gone undiagnosed too long.
So, there is a double-edged sword with regard to pain medicine. On one hand it can make real issues like GB disease, either infection, or with calculi, go undiagnosed by covering up the problem.
On the other hand, it can cause the GB, biliary duct, (both to elongate and enlarge) and the Oddi to malfunction by having had taken opioid pain medicine.
How does one distinguish between the differences?
One: simple Physician-patient exam using the hand placed under the right rib-cage while patient inhales fully will give a general yes or no to begin with (at the end of this post I will describe the technique of checking for Murphy's Sign).
Two: Ultra-Sound of right upper quadrant of the abdomen will rule out calculi (stones), and also note the dimensions of the biliary duct (general 1cm or 5-6mm in length normally), the size and dimensions of the GB itself, can vary according to body size but will be noted if larger than expected. The right kidney will also be noted on the exam ( in the report as well).
Three: HIDA scan (a GB function test) will check to see how well it reacts. Whether it stores the bile adequately; and whether it releases it sufficiently. A 70%+ is generally normal.
NOW, with all this information in hand.
Rule out calculi...
Rule out infection... (if possible)
Are you on opioids...
If you can say NO..NO..Yes... Then you may have several or more options without having to have surgery. Some of which will be effective within a week to 10 days maximum.
You taper off opioids and transition to another pain medicine(s): for example TalwinNX (pentazocine with Naloxone) is effective for mild to severe pain; and has no known effect (positive or negative) on the GB or hepatic system as a whole.
Start taking Ketoprofen (is an NSAID similar family as Ibuprofen) either 50 or 100mg capsules. Is 'very' effective in pain relief, and has an anti-inflammatory effect to help any irritation from the enlarged GB and constituent parts.
IN concert these two can work wonderfully for pain relief, most often MUCH better than the opioid counterparts.
If you have calculi you can have them removed without having the whole GB removed. Better alternative.
Switching medication from opioids rather than have a GB removal is preferable as well.
The side-effects from post-surgery GB removal can include transient 'dumping syndrome' (the bile dumps into duodenum and runs through you quickly) OFTEN, and in most cases this lasts only a few months or a few weeks, until your body adjusts.
Some pain at surgery site is common up to several months as it all heals and adjusts.
There are many other complications that can occur, however we are looking to avoid the surgery in general!
SO, THOSE with "Opioid Induced Hypo-functional Gallbladder disease" and not knowing it, can have relief, as well as alternate options.
------How to check for Murphy's Sign-----
These symptoms can often mask themselves as many things. The over-all symptoms are often so general they can easily be over-looked Or OVER-diagnosed.
A SIMPLE examination (prelim) that a physician can or SHOULD do when even the gallbladder is suspected is the test for Murphy's Sign.
If you've had it you'll remember. If you were positive for Murphy's sign you'll Certainly Remember! Is as follows and can be done with a partner.
Patient laying down- physician takes index through ring finger and gently places them just under the right rib cage one hand span away from middle of center front to a depth of one-two inches down and UP under the ribs. Patient takes a deep breath semi-quickly.
IF there is SEVERE BLINDING PAIN and patient cannot continue to inhale----POSITIVE MUPRHY'S SIGN, one takes step 2 .Ultra sound and/OR--.HIDA SCAN
IF there is only general discomfiture NEGATIVE--- Ultra Sound, perhaps HIDA scan still advisable under discretion of other symptoms.
--------------------------Lastly a bit of history on the Hepatic system------------------
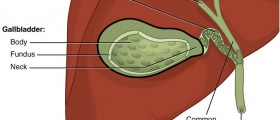
The gallbladder is part of a large number of organs that work in concert with one another: The liver (produces bile, and enzymes, besides being the 2nd largest organ in your body, after your skin), the gallbladder (stores said enzymes waiting for a signal to release into duodenum just below stomach/into stomach), to biliary duct (which receives , or transceives the bile enzymes), to the sphincter of Oddi (which opens and closes letting out the bile into duodenum(small intestine below stomach)).
Symptoms of a gallbladder attack caused by disease, stones, enlarged biliary duct, or malfunctioning of the Oddi can be caused by numerous stimuli.
A very common, but UNDER-diagnosed cause of non-calculi (meaning no stones) gallbladder enlargement can be from taking prescription pain medication. The duct is enlarged, the gallbladder is enlarged, and upon having a HIDA scan (a routine gallbladder function test) you have a hypo-active gallbladder (under active) the cause may simply be the opioid pain medicine. Many people have been told to have surgery with that being the cause.
SYMPTOMS: common and uncommon of ALL types of hypo-active gallbladder can be from pain after meals, any -- or none.
--Severe headache generally located at top of head.
--Mild to severe pain in abdomen, from right-center, upper OR lower to left side of abdomen as well.
--mild to severe pain in the back and/or side, to between right and/or left shoulder blades. can radiate to upper shoulder down to lower abdomen right side of trunk to middle.
--mild to Severe nausea after eating or drinking fatty, non-fatty foods. Drinking coffee, alcohol, heavy juices causing a stabbing pain on right central side to upper middle chest.
These symptoms can often mask themselves as many things. The over-all symptoms are often so general they can easily be over-looked Or OVER-diagnosed.
------------------------------Good Luck------------------------
The Oddi is what opens and closes to let the bile enter the duodenum (small intestine traversing just below the stomach).
(BELOW, at end is a short but comprehensive explanation of the Hepatic system with Gallbladder and functions)
Persons who have Gallbladder (from here on will be noted as GB) issues AND are taking opioid pain medication (i.e. any morphine based/derived product-- percocet, dilaudid, vicodin, morphine, etc... any drug derived from the poppy plant (known as an opiate, e.g. opioid (meaning opiate-like)) may not need surgery.
Here lies the reason:
Opioids cause a number of bodily effects, from pain relief to elongating the intestine (hence causing constipation) to making the GB and its parts react slowly or lazily.
In tests done persons having had HIDA scans done (in real time) were injected with Naloxone (Narcan, an 'anti-opioid') had thier GB's and the Oddi go from little to no function-- to fully functional within a span of several minutes or less.
The patient had GB problems, and took opioid pain medication as well. When the opioid effect was removed the GB function was restored fully, or nearly so.
There is, and can be, a viscious cycle with regards to this.
For example, a person takes pain medicine for one reason, the medicine can cause GB issues, which causes pain. The patient takes more medication for the pain, causing the GB issues to worsen, and so on.
Conversely, a person with GB issues who starts taking opioid pain medication can mask the pain for a while, thus allowing it to go undiagnosed for a span of time until it becomes too pernicious to avoid, therefore needing surgery because a rupture from distention of the GB and biliary duct (either with calculi (gall-stones: made of calcium, magnesium, sodiums, etc)) from having gone undiagnosed too long.
So, there is a double-edged sword with regard to pain medicine. On one hand it can make real issues like GB disease, either infection, or with calculi, go undiagnosed by covering up the problem.
On the other hand, it can cause the GB, biliary duct, (both to elongate and enlarge) and the Oddi to malfunction by having had taken opioid pain medicine.
How does one distinguish between the differences?
One: simple Physician-patient exam using the hand placed under the right rib-cage while patient inhales fully will give a general yes or no to begin with (at the end of this post I will describe the technique of checking for Murphy's Sign).
Two: Ultra-Sound of right upper quadrant of the abdomen will rule out calculi (stones), and also note the dimensions of the biliary duct (general 1cm or 5-6mm in length normally), the size and dimensions of the GB itself, can vary according to body size but will be noted if larger than expected. The right kidney will also be noted on the exam ( in the report as well).
Three: HIDA scan (a GB function test) will check to see how well it reacts. Whether it stores the bile adequately; and whether it releases it sufficiently. A 70%+ is generally normal.
NOW, with all this information in hand.
Rule out calculi...
Rule out infection... (if possible)
Are you on opioids...
If you can say NO..NO..Yes... Then you may have several or more options without having to have surgery. Some of which will be effective within a week to 10 days maximum.
You taper off opioids and transition to another pain medicine(s): for example TalwinNX (pentazocine with Naloxone) is effective for mild to severe pain; and has no known effect (positive or negative) on the GB or hepatic system as a whole.
Start taking Ketoprofen (is an NSAID similar family as Ibuprofen) either 50 or 100mg capsules. Is 'very' effective in pain relief, and has an anti-inflammatory effect to help any irritation from the enlarged GB and constituent parts.
IN concert these two can work wonderfully for pain relief, most often MUCH better than the opioid counterparts.
If you have calculi you can have them removed without having the whole GB removed. Better alternative.
Switching medication from opioids rather than have a GB removal is preferable as well.
The side-effects from post-surgery GB removal can include transient 'dumping syndrome' (the bile dumps into duodenum and runs through you quickly) OFTEN, and in most cases this lasts only a few months or a few weeks, until your body adjusts.
Some pain at surgery site is common up to several months as it all heals and adjusts.
There are many other complications that can occur, however we are looking to avoid the surgery in general!
SO, THOSE with "Opioid Induced Hypo-functional Gallbladder disease" and not knowing it, can have relief, as well as alternate options.
------How to check for Murphy's Sign-----
These symptoms can often mask themselves as many things. The over-all symptoms are often so general they can easily be over-looked Or OVER-diagnosed.
A SIMPLE examination (prelim) that a physician can or SHOULD do when even the gallbladder is suspected is the test for Murphy's Sign.
If you've had it you'll remember. If you were positive for Murphy's sign you'll Certainly Remember! Is as follows and can be done with a partner.
Patient laying down- physician takes index through ring finger and gently places them just under the right rib cage one hand span away from middle of center front to a depth of one-two inches down and UP under the ribs. Patient takes a deep breath semi-quickly.
IF there is SEVERE BLINDING PAIN and patient cannot continue to inhale----POSITIVE MUPRHY'S SIGN, one takes step 2 .Ultra sound and/OR--.HIDA SCAN
IF there is only general discomfiture NEGATIVE--- Ultra Sound, perhaps HIDA scan still advisable under discretion of other symptoms.
--------------------------Lastly a bit of history on the Hepatic system------------------
The gallbladder is part of a large number of organs that work in concert with one another: The liver (produces bile, and enzymes, besides being the 2nd largest organ in your body, after your skin), the gallbladder (stores said enzymes waiting for a signal to release into duodenum just below stomach/into stomach), to biliary duct (which receives , or transceives the bile enzymes), to the sphincter of Oddi (which opens and closes letting out the bile into duodenum(small intestine below stomach)).
Symptoms of a gallbladder attack caused by disease, stones, enlarged biliary duct, or malfunctioning of the Oddi can be caused by numerous stimuli.
A very common, but UNDER-diagnosed cause of non-calculi (meaning no stones) gallbladder enlargement can be from taking prescription pain medication. The duct is enlarged, the gallbladder is enlarged, and upon having a HIDA scan (a routine gallbladder function test) you have a hypo-active gallbladder (under active) the cause may simply be the opioid pain medicine. Many people have been told to have surgery with that being the cause.
SYMPTOMS: common and uncommon of ALL types of hypo-active gallbladder can be from pain after meals, any -- or none.
--Severe headache generally located at top of head.
--Mild to severe pain in abdomen, from right-center, upper OR lower to left side of abdomen as well.
--mild to severe pain in the back and/or side, to between right and/or left shoulder blades. can radiate to upper shoulder down to lower abdomen right side of trunk to middle.
--mild to Severe nausea after eating or drinking fatty, non-fatty foods. Drinking coffee, alcohol, heavy juices causing a stabbing pain on right central side to upper middle chest.
These symptoms can often mask themselves as many things. The over-all symptoms are often so general they can easily be over-looked Or OVER-diagnosed.
------------------------------Good Luck------------------------
Loading...
With regard to my above posting:
I am willing to take questions, offer opinions, and help in any way I am capable. My expertise in diagnosing difficult symptoms that include many other areas of the body are somewhat extensive-- and would be my pleasure to.
My goal has always been to educate, inform, and treat with care all persons regardless of whether another physician believes them or has been helpful.
It is unfortunate that in the current medical environment that physicians have 'over-booked' their patients, and cannot spend the time necessary to simply 'think' about one thing or another. ALSO, the reluctance for them to 'look-up' something that they either have forgotten-- treated less to never, or re-educate to educate themselves on less understood areas is all too common.
The truth is most physicians don't have the time. Second, they don't want to admit they may need to refer back to the basics.
And MOST important, and all too true: Most Doctors have too much information 'crammed' into the heads that they are now limited in diagnoses beyond the 'routine standard' if this then that standard protocol.
It is unfortunate. But is it unfortunately true.
I have a joke that is not meant to be funny, but meant to make one 'think'.... And is as follows:
Q- "What do you call a doctor who graduates at the bottom of their class??..."
A- "A Doctor."
Let it sink in, and you will realize the truth... We are all human. And are not required to be in the top 5 percentile to become a physician.
Aww... One more joke, but very accurate; though has to do with another subject; as follows:
Q- "How many psychologists does it take to change a lightbulb?"
A- "One. But the lightbulb has to 'want' to change."
Again too true. (think how hard it is to change yourself, and then realize what little chance you have of changing someone else.)
Well, if you wish to ask questions; please include symptoms, causes (if known), medications taken (and what for; not all are prescribed for given reasons). History, procedures in the past, work, diet, exercise, etc...along with age, gender, smoking/drinking habits--(be honest pls, otherwise I cannot help as much).
Family history is not outside the helpful realm either...DId anyone have similar problems in the past etc... Did you travel outside the country, to Asia, India, to the USA... Often the most mundane detail can be the most important.
Thanks, and Good health all...
I am willing to take questions, offer opinions, and help in any way I am capable. My expertise in diagnosing difficult symptoms that include many other areas of the body are somewhat extensive-- and would be my pleasure to.
My goal has always been to educate, inform, and treat with care all persons regardless of whether another physician believes them or has been helpful.
It is unfortunate that in the current medical environment that physicians have 'over-booked' their patients, and cannot spend the time necessary to simply 'think' about one thing or another. ALSO, the reluctance for them to 'look-up' something that they either have forgotten-- treated less to never, or re-educate to educate themselves on less understood areas is all too common.
The truth is most physicians don't have the time. Second, they don't want to admit they may need to refer back to the basics.
And MOST important, and all too true: Most Doctors have too much information 'crammed' into the heads that they are now limited in diagnoses beyond the 'routine standard' if this then that standard protocol.
It is unfortunate. But is it unfortunately true.
I have a joke that is not meant to be funny, but meant to make one 'think'.... And is as follows:
Q- "What do you call a doctor who graduates at the bottom of their class??..."
A- "A Doctor."
Let it sink in, and you will realize the truth... We are all human. And are not required to be in the top 5 percentile to become a physician.
Aww... One more joke, but very accurate; though has to do with another subject; as follows:
Q- "How many psychologists does it take to change a lightbulb?"
A- "One. But the lightbulb has to 'want' to change."
Again too true. (think how hard it is to change yourself, and then realize what little chance you have of changing someone else.)
Well, if you wish to ask questions; please include symptoms, causes (if known), medications taken (and what for; not all are prescribed for given reasons). History, procedures in the past, work, diet, exercise, etc...along with age, gender, smoking/drinking habits--(be honest pls, otherwise I cannot help as much).
Family history is not outside the helpful realm either...DId anyone have similar problems in the past etc... Did you travel outside the country, to Asia, India, to the USA... Often the most mundane detail can be the most important.
Thanks, and Good health all...
Loading...
I really want to thank you for posting this. This is exactly what's been causing my GB pain all along. Originally I had GB problems and was diagnosed with GB dyskinesia in 2006 and as I recall I was taking Percocet when it started back then too. I went to the ER and they gave me morophine, which made my pain way worse after it wore off. They did the usual GB tests and when it came back 6%, surgery was advised but I refused and it got better over a long period of time. Just recently, I had been taking Lortab for a condition and last Saturday my GB pain started again (about a half hour after taking the Lortab, right as the effect of the med started to kick in). Every last symptom is like it was before, which is exactly as you describe and because the pain first presented itself as the med took effect, I'm positive it's this. After reading this I'm going to get away from opioid-based meds. Other than that, is there anything else I can do to aid my recovery? Should I ask about Naloxone? Again, I thank you so much for sharing this information.
Loading...
Naloxone (or NARCAN) by itself NO. It is used for anesthesia recovery, or for over-dose patients. It is an opioid antangonist.
It blocks the mui receptors in the brain (which are the same ones that 'accept' the opioid to have it be effective).
Long story short on Narcan/Naloxone.... In concert with another drug like pentazocine ORALLY ONLY it has a metabolic rate different than taken in the hospital parentally (I.V.)
So...NO.... Do not ask for Naloxone/Narcan as a relief measure... In TalwinNX it is very effective, ecause the 2 different drugs metabloize at different rates causing an effect that for 'pentazocine alone' would only be for mild pain, instead is for moderate to severe...
Narcan will put a patient who is dependent on narcotic pain medicine into INSTANT withdrawal. Which is also why it is used to help Over-Dose patients, AND used to aid in anesthesia recovery.
There are other options though...
Ketoprofen (was over the counter, isnt any more; because of marketing not side-effect issues whatsoever) is very effect in pain relief.
Most notably Dentists use it and goes by the Brand name of Orudis and Oravale (50 or 100mg casule)
In my experience ketoprofen works much better than ibuprofen all the way around...
A combination of that with Talwin...Pentazocine alone (not the NX) or a number of other non-narcotic drugs can do the trick...and do it VERY WELL... often better than narcotics often!
Sorry if I led you to a confusion of the Narcan/Naloxone... Again, by itself? Is not prescribed for above said reasons...
Thanks.
It blocks the mui receptors in the brain (which are the same ones that 'accept' the opioid to have it be effective).
Long story short on Narcan/Naloxone.... In concert with another drug like pentazocine ORALLY ONLY it has a metabolic rate different than taken in the hospital parentally (I.V.)
So...NO.... Do not ask for Naloxone/Narcan as a relief measure... In TalwinNX it is very effective, ecause the 2 different drugs metabloize at different rates causing an effect that for 'pentazocine alone' would only be for mild pain, instead is for moderate to severe...
Narcan will put a patient who is dependent on narcotic pain medicine into INSTANT withdrawal. Which is also why it is used to help Over-Dose patients, AND used to aid in anesthesia recovery.
There are other options though...
Ketoprofen (was over the counter, isnt any more; because of marketing not side-effect issues whatsoever) is very effect in pain relief.
Most notably Dentists use it and goes by the Brand name of Orudis and Oravale (50 or 100mg casule)
In my experience ketoprofen works much better than ibuprofen all the way around...
A combination of that with Talwin...Pentazocine alone (not the NX) or a number of other non-narcotic drugs can do the trick...and do it VERY WELL... often better than narcotics often!
Sorry if I led you to a confusion of the Narcan/Naloxone... Again, by itself? Is not prescribed for above said reasons...
Thanks.
Loading...
Since I cannot edit my posts I need to clarify or condense what I said above... You scared me with the Narcan thought so I wrote fast.
You will only find it in TalwinNX, no other oral drug (that I'm aware of) contains Narcan.
Pentazocine by itself is SO-so in pain relief, BUT is non-narcotic, and won't affect the hepatic system.
When mixed with Naloxone the potent quality almost 'doubles' or more.
Ketoprofen is fantastic, they lacked a huge marketing team, and armies of drug-Reps so it is relatively unknown to the public. It lasts for 12hours per dose, and works 'Wonderful' for pain relief. I use it instead of OTC Ibuprofen becuase it is fantastic.
One needs not have Naloxone to fix opioid induced GB issues. Just either lower the dosage of opioids+add ketoprofen (or the like), or taper off opioids and use ketoprofen (or the like) instead, or use other options in concert with each other as stated above.
No physician will prescribe Narcan alone to a patient... IF they do, they should be stripped of thier medical license.
I hope this helps.
You will only find it in TalwinNX, no other oral drug (that I'm aware of) contains Narcan.
Pentazocine by itself is SO-so in pain relief, BUT is non-narcotic, and won't affect the hepatic system.
When mixed with Naloxone the potent quality almost 'doubles' or more.
Ketoprofen is fantastic, they lacked a huge marketing team, and armies of drug-Reps so it is relatively unknown to the public. It lasts for 12hours per dose, and works 'Wonderful' for pain relief. I use it instead of OTC Ibuprofen becuase it is fantastic.
One needs not have Naloxone to fix opioid induced GB issues. Just either lower the dosage of opioids+add ketoprofen (or the like), or taper off opioids and use ketoprofen (or the like) instead, or use other options in concert with each other as stated above.
No physician will prescribe Narcan alone to a patient... IF they do, they should be stripped of thier medical license.
I hope this helps.
Loading...
I misunderstood and thought you meant Narcan could help recover opioid related GB dysfunction. I didn't mean for for pain relief. I've had this problem before but didn't understand what caused it until I read this post and remembered being on opioids when it happened the last time. When it happened this time it began directly after using Lortab, a telltale sign. My doctor advised surgery but I refused because I have IBS and I worry about the potential GI problems GB removal might cause in a patient who already has GI issues. I did recover from this before w/o surgery but it took almost two years, which is why I asked about Narcan. During my past experience with this I had two hidascans--one was 6% when I started having problems and 61% when I was recovering. I appreciate your post and taking time to answer my questions.
Loading...
Hey, no problem... I can see how it is almost contradictory in nature. During a study of persons during HIDA some Doc decided to dose them with narcan to see if that will affect the Oddi, and lo-and-behold it did. Thus proving the opioid effect on it the test results.
He published it in the AJM in '91 oct I think... but, if I could revamp my supposition above to clarify I would, but it does give one hope and options versus surgery...
Personally I think you made a wonderfully informative, or very intuitive decision with regards to IBS and GB surgery as well..
Few people will say 'No' to the Doc on these things, hence too many unneeded removals happen... Hey, good luck, and I am very glad it helped, or helps...!!!
Samuel
He published it in the AJM in '91 oct I think... but, if I could revamp my supposition above to clarify I would, but it does give one hope and options versus surgery...
Personally I think you made a wonderfully informative, or very intuitive decision with regards to IBS and GB surgery as well..
Few people will say 'No' to the Doc on these things, hence too many unneeded removals happen... Hey, good luck, and I am very glad it helped, or helps...!!!
Samuel
Loading...
Hey, I know this post is nearly a month old and I don't know if the OP sees it anymore but I just wanted to let you know I took your advice and stayed away from opioids and I'm doing much better today. Thank you again for helping me and hope you have a good holiday.
Chuck
Chuck
Loading...
I understand that this post is over two years old but this is the first time I have felt that I have had any clarification as to what I am experiencing. I am desperate to contact Sawyl and I am hoping you are notified of this post. I am having gallbladder issues and I have some questions.
Loading...
Hi, I'm a 23 year old male. I don't exercise very frequently...maybe 2 times a week, some days I drink 1-2 alcoholic beverages but very rarely do I make it a habit, I've smoked since I was 18 except now I smoke here and there. When I do I don't smoke more than 3 cigarettes a day. Right now I've been smoke free for a week and counting. My diet consists of mainly healthy stuff. I haven't been out to eat fast food in quite a long time due to problems like acid reflux, or what I thought was acid reflux.
A couple months ago I had to go to the ER because of intense abdominal pain. The pain usually starts below my sternum. It's this dull ACHING pain that slowly gets worse and worse. The pain usually lasts hours. My longest attack lasted 8 hours and my shortest attack lasted 15 minutes. The first time I had an attack was over a year ago; back then they wouldn't last very long. As time has gone by the pain has gotten worse and has lasted longer. I also notice that I get pain around my chest and between my shoulder blades, most notably on the left side (both chest and shoulder).
Anyways, I went to the ER and they gave me some medicine that they thought would alleviate my pain and also scheduled me for an ultrasound. The doctor was quite sure that I had IBS and prescribed me some Librax which would help with the pain. It didn't though. The next day I went in for an ultrasound and found out I had gallstones and that the pain I have been experiencing may very well be related to the gallstones I have. Since then I have set up surgery to get rid of my gallbladder.
There are so many times, though, when I wonder whether or not it could actually be my gallbladder bothering me. I can't help but to go between acid reflux and gallstones for the cause of my pain...Like I said, I have changed my eating habits a lot. I don't drink any carbonated drinks, I don't eat out at fast food restaurants (the only place I'm comfortoable eating at is Subway), when I eat meat I only eat lean meats like turkey breast or chicken breast, I don't eat any cheese at all, in the mornings my breakfast consists of fat free lactose free milk with cereals that are low in fat and wheat bread or a wheat bagel with a little bit of fruit spread. Throughout the day I usually snack on things like fat free pretzels, dry cereal (raisin bran for fiber) and for a meal I usually have steamed white rice with veggies like cabbage, cucumbers, yucca, brocolli, cauliflower, carrots etc. I also try not to overeat on top of being so careful with what I eat. I don't eat too close to bedtime (I usually don't eat within 5 hours of when I go to sleep) and I sleep upright at night in fear that I may have a painful acid reflux attack at night.
Even with all these precautions I still have painful attacks here and there that seem to come unprovoked. Today I drank a Red Bull in the morning and lo and behold 4 hours later I was in pain. It could've been that or the fact that I may have overeaten or eaten to fast today. I just can't pinpoint why I'm having these attacks but I was hoping that someone as knowledgeable as you may be able to help me or give me some insight as to what you think the problem is.
Also, I've been taking hydrocodone/APAP 5/325 for pain until my surgery comes up. If I feel an attack coming on I usually take one and I'm good as far as pain goes. Sometimes if I don't take it soon enough the pain pill won't do much and I'll experience an attack Although last time I had an attack I took 3 pills (2 at first, then 1 an hour later) the attack was cut to 4 hours instead of the usual 8 hours. Still VERY unpleasant. Like I said, the pain pills help but only if I'm able to pinpoint when an attack is going to come on; if I don't take them on time, the attack comes but lasts less.
I don't know if these symptoms are characteristic of reflux, IBS or gallstones (I myself am leaning towards gallstones....but only in hopes that the removal of it will help me get rid of the pain). I have looked into liver flushes and I have to say that I'm not interested in them by the way. If you decide to reply, I would appreciate that so much. ***this post is edited by moderator *** *** private e-mails not allowed*** Please read our Terms of Use
A couple months ago I had to go to the ER because of intense abdominal pain. The pain usually starts below my sternum. It's this dull ACHING pain that slowly gets worse and worse. The pain usually lasts hours. My longest attack lasted 8 hours and my shortest attack lasted 15 minutes. The first time I had an attack was over a year ago; back then they wouldn't last very long. As time has gone by the pain has gotten worse and has lasted longer. I also notice that I get pain around my chest and between my shoulder blades, most notably on the left side (both chest and shoulder).
Anyways, I went to the ER and they gave me some medicine that they thought would alleviate my pain and also scheduled me for an ultrasound. The doctor was quite sure that I had IBS and prescribed me some Librax which would help with the pain. It didn't though. The next day I went in for an ultrasound and found out I had gallstones and that the pain I have been experiencing may very well be related to the gallstones I have. Since then I have set up surgery to get rid of my gallbladder.
There are so many times, though, when I wonder whether or not it could actually be my gallbladder bothering me. I can't help but to go between acid reflux and gallstones for the cause of my pain...Like I said, I have changed my eating habits a lot. I don't drink any carbonated drinks, I don't eat out at fast food restaurants (the only place I'm comfortoable eating at is Subway), when I eat meat I only eat lean meats like turkey breast or chicken breast, I don't eat any cheese at all, in the mornings my breakfast consists of fat free lactose free milk with cereals that are low in fat and wheat bread or a wheat bagel with a little bit of fruit spread. Throughout the day I usually snack on things like fat free pretzels, dry cereal (raisin bran for fiber) and for a meal I usually have steamed white rice with veggies like cabbage, cucumbers, yucca, brocolli, cauliflower, carrots etc. I also try not to overeat on top of being so careful with what I eat. I don't eat too close to bedtime (I usually don't eat within 5 hours of when I go to sleep) and I sleep upright at night in fear that I may have a painful acid reflux attack at night.
Even with all these precautions I still have painful attacks here and there that seem to come unprovoked. Today I drank a Red Bull in the morning and lo and behold 4 hours later I was in pain. It could've been that or the fact that I may have overeaten or eaten to fast today. I just can't pinpoint why I'm having these attacks but I was hoping that someone as knowledgeable as you may be able to help me or give me some insight as to what you think the problem is.
Also, I've been taking hydrocodone/APAP 5/325 for pain until my surgery comes up. If I feel an attack coming on I usually take one and I'm good as far as pain goes. Sometimes if I don't take it soon enough the pain pill won't do much and I'll experience an attack Although last time I had an attack I took 3 pills (2 at first, then 1 an hour later) the attack was cut to 4 hours instead of the usual 8 hours. Still VERY unpleasant. Like I said, the pain pills help but only if I'm able to pinpoint when an attack is going to come on; if I don't take them on time, the attack comes but lasts less.
I don't know if these symptoms are characteristic of reflux, IBS or gallstones (I myself am leaning towards gallstones....but only in hopes that the removal of it will help me get rid of the pain). I have looked into liver flushes and I have to say that I'm not interested in them by the way. If you decide to reply, I would appreciate that so much. ***this post is edited by moderator *** *** private e-mails not allowed*** Please read our Terms of Use
I hope that this message reaches you well and that you can help me and give me some more insight on these problems that I'm having. Thank you for sitting through this :)
Loading...
I would also like to add that within the last month I have developed a new "symptom". About a bit over half of the time I have a bowel movement I have mucus in my stool. The mucus is very noticeable, it is usually clumps of mucus that are attached to the stool. I have normal bowel movements, though. I'm not constipated and don't have diarrhea. This month, though, I did have diarrhea for no real apparent reason (well maybe because I traveled) that lasted for about a week but other than that I'm quite normal with bowel movements.
One last thing! Over a month ago I underwent treatment for the erradication of h. pylori, which I tested having antibodies for. I am still waiting to get re-tested.
One last thing! Over a month ago I underwent treatment for the erradication of h. pylori, which I tested having antibodies for. I am still waiting to get re-tested.
Loading...
I'm glad you posted this information. I have had some very unusual symptoms but the only thing they could find wrong was my gallbladder and was dx'd with biliary dyskonesia. I had my gallbladder removed a week ago. My symptoms were unexpected weight loss (I went from 125 to 103 lbs within a few months), chronic constipation, random stomach pains (but never in the gallbladder area) and then I started having mouth swelling and sores. I have been on and off narcotics over the ears due to sports injuries, orthopedic surgeries, arthritis, back pain. I worked out regularly. When my gallbladder was removed, doc said it was very diseased. I'm still on narcs due to post surgical pain and my normal joint pains. However I have been eating much better the last couple of days. Have you ever heard of such symptoms related to gallbladder disease? The only other "normal" sx's I've experienced were the gas, bloating etc. Very little acid reflux. I've heard that biliary dyskonesia is often a symptom of another problem, so I am worried about other issues that I may have. Any input would be appreciated if you have the time. Thank you!
Loading...
sawyl.... is there any way i can contact you. I really need help and have been suffering for so long. Your post sounds like it may be very close to what has been destroying my life
Loading...
WOW,, I am reading more of your posts and alot of this makes sense, a few years ago i read about suboxone (wich contains naloxone) for pain treatment. I asked to go on it as an alternative to opiod medication because i couldn't take the foggy feeling anymore, and for the most part it works to treat the pain. If what your saying is true, quite possibly the naloxone in the subox is what is giving me relief? I really wish i could speak with you directly
Loading...