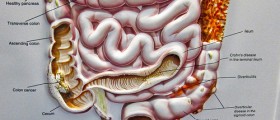
Had an issue of intermittent incomplete rectal emptying. Was diagnosed with a sigmoidocele on a defecogram. Was told by 3 colorectal surgeons I needed my sigmoid colon removed. The operating colorectal surgeon removed my sigmoid colon but additionally removed the top of my rectum (which I did not and would not have consented to as there was no diseased tissue.) Multiple other procedures were done (many beyond consent) on healthy tissues that had no connection with my presenting symptom. (Operating GYN did a resuspension of vaginal vault that was not prolapsing, "repair" of tiny asymptomatic cystocele (resulting in bladder overcorrection), removal of functioning left ovary along with right ovary that had a 4 inch benign simple cyst, "repair" of a very small rectocele never examined by either of the two operating surgeons). The operating surgeons got paid per procedure and each got paid a percentage to assist the other.
3 weeks post-op I developed a severe stricture (narrowing) at the anastomosis where what was left of my rectum was joined to a bit of sigmoid that was left. The narrowed my colon to only 4 millimeters in diameter. The surgeon diagnosed this by gastrograffin xray but said he would "do nothing about it." I had to seek my own help. In a month a neighbor drove me to an ER of a top city hospital 100 miles from my home. They arranged emergent dilations with one of their surgeons. After only 2 dilations, the stricture stayed open, but the walls of the colon were scarred intrinsically and that part of my colon was no longer muscular (had no peristaltic ability). The ischemia (lack of blood flow) then spread along a 4-inch stretch of my colon and that was non-peristaltic. Scarring of my levator ani pelvic floor muscle then prevented my puborectalis muscle from allowing my rectum to straighten for defecation as it could prior to the low anterior resection. In addition to now not being able to defecate, I also could not eat due to on-going small bowel obstructions caused by dense scarring that formed around my distal ileum just over what was left of my rectum.
It took 13 months of seeing 11 doctors at 7 medical centers before all of the complications could be diagnosed. The next challenge was finding a surgeon with the skill and willingness to address all of this damage. Luckily I found one. What had to be done to save my life was an extensive lysis of adhesions on my small intestine and a permanent ileostomy. I now pass waste out of my small intestine into a bag. However, I am grateful to be alive.
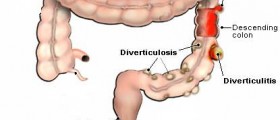
Upon review of my case, it was found by 4 pelvic radiology reviewers that I did not have a sigmoidocele in the first place. A resident radiologist apparently thought it was my sigmoid colon that temporarily internally prolapsed through a space between the top of my rectum and the top of my vagina only at the "push" phase of the test then returned to normal position. In reality, it was only a loop of small intestine. Further this transient internal prolapse of the loop of small intestine did not happen until I had already passed the rectal contrast so did not hinder rectal emptying. Surgery for this would not have included any colon resection but instead just closure of the space through which the small intestine internally herniated. This could have been done vaginally.
The real cause of my intermittent incomplete rectal empyting was never adequately diagnosed as many standard tests were never done prior to surgery. These include anorectal manometry, pudental nerve terminal latency tests, transit tests, EMG studies. I did not know of these at the time so did not know to ask for them. None of the 3 colorectal surgeons I consulted with recommended them. These tests could have diagnosed some issue with the function of my pelvic muscles or nerves that did not indicate surgery or may have indicated a condition that would be made worse by surgery.
Inadequate pre-op testing, misdiagnosis of testing that was done, wrong surgery performed with many additional procedures not connected to presenting symptom, and no follow-up to complications were what I experienced and are the basis for current litigation. That was my experience with low anterior resection.
3 weeks post-op I developed a severe stricture (narrowing) at the anastomosis where what was left of my rectum was joined to a bit of sigmoid that was left. The narrowed my colon to only 4 millimeters in diameter. The surgeon diagnosed this by gastrograffin xray but said he would "do nothing about it." I had to seek my own help. In a month a neighbor drove me to an ER of a top city hospital 100 miles from my home. They arranged emergent dilations with one of their surgeons. After only 2 dilations, the stricture stayed open, but the walls of the colon were scarred intrinsically and that part of my colon was no longer muscular (had no peristaltic ability). The ischemia (lack of blood flow) then spread along a 4-inch stretch of my colon and that was non-peristaltic. Scarring of my levator ani pelvic floor muscle then prevented my puborectalis muscle from allowing my rectum to straighten for defecation as it could prior to the low anterior resection. In addition to now not being able to defecate, I also could not eat due to on-going small bowel obstructions caused by dense scarring that formed around my distal ileum just over what was left of my rectum.
It took 13 months of seeing 11 doctors at 7 medical centers before all of the complications could be diagnosed. The next challenge was finding a surgeon with the skill and willingness to address all of this damage. Luckily I found one. What had to be done to save my life was an extensive lysis of adhesions on my small intestine and a permanent ileostomy. I now pass waste out of my small intestine into a bag. However, I am grateful to be alive.
Upon review of my case, it was found by 4 pelvic radiology reviewers that I did not have a sigmoidocele in the first place. A resident radiologist apparently thought it was my sigmoid colon that temporarily internally prolapsed through a space between the top of my rectum and the top of my vagina only at the "push" phase of the test then returned to normal position. In reality, it was only a loop of small intestine. Further this transient internal prolapse of the loop of small intestine did not happen until I had already passed the rectal contrast so did not hinder rectal emptying. Surgery for this would not have included any colon resection but instead just closure of the space through which the small intestine internally herniated. This could have been done vaginally.
The real cause of my intermittent incomplete rectal empyting was never adequately diagnosed as many standard tests were never done prior to surgery. These include anorectal manometry, pudental nerve terminal latency tests, transit tests, EMG studies. I did not know of these at the time so did not know to ask for them. None of the 3 colorectal surgeons I consulted with recommended them. These tests could have diagnosed some issue with the function of my pelvic muscles or nerves that did not indicate surgery or may have indicated a condition that would be made worse by surgery.
Inadequate pre-op testing, misdiagnosis of testing that was done, wrong surgery performed with many additional procedures not connected to presenting symptom, and no follow-up to complications were what I experienced and are the basis for current litigation. That was my experience with low anterior resection.
Loading...