:(
This may be in the wrong category & I do apologize if it is.
I'm a 54-yr old female who has not had many medical maladies in her lifetime except bronchitis occasionally, with the exception of being diagnosed with mild mitral valve regurgitation in 1997.
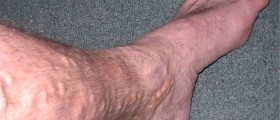
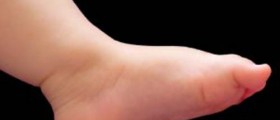
However, for over two months now I have had these ugly red/purple swollen feet & legs (six inches below the knee and downward all around the leg) that are extremely painful, hard to walk and sometimes I cannot wear shoes or socks because of it; or if I do it is short term wear because of the pain. It hurts for anything to even brush up against them. 90% of the time I must go barefooted just to be even a bit comfortable. There have been no skin breakage or lesions with this, but my feet now have 'stretch marks' from all the swelling.
I simply woke up one day to go to work as normal and these symptoms were present. I've never experienced anything like this before.
I've been to the ER twice since this started in early February. First time, I was diagnosed with cellulitis, but there was no response to several rounds of very expensive antibiotic treatments, yet the swelling persists. Second time to the ER, 3 weeks later, doctors thought I may have clots or even DVT. I was admitted and put through rigorous testings, and blood work-ups & was assigned to a pulmonologist. All was normal. The only notation I can make here is that after doing a ct scan they found that I had extremely enlarged lymph nodes in my medialstinum area. A PET scan was then ordered, which came back normal. A sleep study was done where I've learned that I have sleep apnea, i.e. I quit breathing over 60 times in two hours. The only final diagnosis I came out of the hospital with is COPD, with 50% capacity. I am now on oxygen at home, as needed.
The only true relief I get is to lie down in a horizontal position with my feet & legs elevated. After several hours of being horizontal, such as sleep time, the swelling will go down to almost normal size. However, once I'm vertical again, within 1-2 hours the swelling ensues and the pain returns with a vengeance. The pain is almost unbearable at times. Shooting pains up & down my legs into my hips is often present. Walking then becomes very hard to do (& I now have a walker because of it).
Sometimes when I lay down to take a nap, it feels like I'm rolling over & over or going to fall off the bed, i.e. like I'm spinning. This will last 5 to 10 minutes & is worse if I don't close my eyes. Also, I'm extremely fatigued; my vision is becoming more and more blurred (I see double up & down, not side to side) and my vision has become seriously less acuit; I have trouble sometimes with being too hot or too cold in environments where I should be experiencing the opposite effects; I have severe cramping in my hands at times and cannot hold on to anything. This comes on without warning & nothing I do will make it go away until it's ready to go away; I have occasional charly horse type leg cramps (but no restless legs), and the pain is so severe. It takes forever to get it to go away, it seems. Longer than a normal person would take to walk it out. I'd say they last from 45 minutes to two hours, without fail, when they come on. These "charly horse" cramps can come on anytime but usually are while sleeping.
NOW . . . we are back to square one. The several doctors I've been to are completely stumped. They have no clue what this may be. I've been off work now for over 3 months & I need to get back to work, but can't without being able to wear shoes & socks, & of course, to be able to walk normally.
Please help. Do you know what this could possibly be??? Can you give me some ideas or avenues to persue on this issue?
THANK YOU, in advance.
(*Everything stated here has been within the knowledge of a variety of doctors).
This may be in the wrong category & I do apologize if it is.
I'm a 54-yr old female who has not had many medical maladies in her lifetime except bronchitis occasionally, with the exception of being diagnosed with mild mitral valve regurgitation in 1997.
However, for over two months now I have had these ugly red/purple swollen feet & legs (six inches below the knee and downward all around the leg) that are extremely painful, hard to walk and sometimes I cannot wear shoes or socks because of it; or if I do it is short term wear because of the pain. It hurts for anything to even brush up against them. 90% of the time I must go barefooted just to be even a bit comfortable. There have been no skin breakage or lesions with this, but my feet now have 'stretch marks' from all the swelling.
I simply woke up one day to go to work as normal and these symptoms were present. I've never experienced anything like this before.
I've been to the ER twice since this started in early February. First time, I was diagnosed with cellulitis, but there was no response to several rounds of very expensive antibiotic treatments, yet the swelling persists. Second time to the ER, 3 weeks later, doctors thought I may have clots or even DVT. I was admitted and put through rigorous testings, and blood work-ups & was assigned to a pulmonologist. All was normal. The only notation I can make here is that after doing a ct scan they found that I had extremely enlarged lymph nodes in my medialstinum area. A PET scan was then ordered, which came back normal. A sleep study was done where I've learned that I have sleep apnea, i.e. I quit breathing over 60 times in two hours. The only final diagnosis I came out of the hospital with is COPD, with 50% capacity. I am now on oxygen at home, as needed.
The only true relief I get is to lie down in a horizontal position with my feet & legs elevated. After several hours of being horizontal, such as sleep time, the swelling will go down to almost normal size. However, once I'm vertical again, within 1-2 hours the swelling ensues and the pain returns with a vengeance. The pain is almost unbearable at times. Shooting pains up & down my legs into my hips is often present. Walking then becomes very hard to do (& I now have a walker because of it).
Sometimes when I lay down to take a nap, it feels like I'm rolling over & over or going to fall off the bed, i.e. like I'm spinning. This will last 5 to 10 minutes & is worse if I don't close my eyes. Also, I'm extremely fatigued; my vision is becoming more and more blurred (I see double up & down, not side to side) and my vision has become seriously less acuit; I have trouble sometimes with being too hot or too cold in environments where I should be experiencing the opposite effects; I have severe cramping in my hands at times and cannot hold on to anything. This comes on without warning & nothing I do will make it go away until it's ready to go away; I have occasional charly horse type leg cramps (but no restless legs), and the pain is so severe. It takes forever to get it to go away, it seems. Longer than a normal person would take to walk it out. I'd say they last from 45 minutes to two hours, without fail, when they come on. These "charly horse" cramps can come on anytime but usually are while sleeping.
NOW . . . we are back to square one. The several doctors I've been to are completely stumped. They have no clue what this may be. I've been off work now for over 3 months & I need to get back to work, but can't without being able to wear shoes & socks, & of course, to be able to walk normally.
Please help. Do you know what this could possibly be??? Can you give me some ideas or avenues to persue on this issue?
THANK YOU, in advance.
(*Everything stated here has been within the knowledge of a variety of doctors).
Loading...
hi, sorry to hear you have been through the mill bit lately. Do you mind if I askwhether you hav been prescribed any diuretics - furosemide for example, combined with the COPD has anyon investigated the possibilities of LVF? (a form of heart failure) some of your symptoms could offer this as a differential diagnosis.... casig
Loading...
Hi Casig, !
No, I don't mind. Sorry I didn't mention the medications. Yes, I'm currently taking Lasix, and was also prescribed that while in the hospital, but things haven't changed much in a month. I swell up; I go to bed, the swelling goes down, I pee all day, the swelling comes back up and the cycle starts all over on a daily basis. Just some days are worse than others. :-(
Actually, I went to a Cardiologist BEFORE I went to the ER the first time in the first week of February, i.e. when I first started having an inkling of swelling in my feet & legs, because my first thoughts were that of heart failure. As a matter of fact, I saw him before they really ballooned up and turned red a week later. However, he never looked at my feet or legs much except to notate that, "Yes, they look "a little swollen", (looking through my socks, mind you... )
Beings that I have an echocardiogram that suggests mitral valve regurgitation, I wanted this re-checked as well. The last echo was about ten years ago. The only thing this current cardiologist really did for me was run a full blood count; in which all he found were normalities; and then he ran another echo which was found that I have 54% regurgitation which is increased from the original 46%, BUT, it is an oddity that he did not respond to the mmHg 84 pressure on my heart, which I'm told by several, including my current pulmonologist, that this is pretty high and that doctor was asking me why the Cardiologist did not act on this. I could only answer, "I don't know. I'm not the doctor".
The Cardiologist told me that he did not hear the usual "murmur" that is normally heard with mitral valve regurgitation or prolapse. I honestly don't know what that means to him. Why the cardiologist did nothing for me at that time, I simply have no clue at this juncture. I went to him because he was highly referred and is considered one of the best in the country. After the visit, he simply referred me to a pulmonologist and then back to my primary for treatment for the legs, which so far, has gone no where.
I have not heard of LVF. But, I'm assuming is probably "Left Ventricular Failure"? Or something like that? You would think with all the poking, sticking, scans, and bloodwork that's been done that CHF or LVF, as you've mentioned, would be looked upon as a possibility. My soonest next appointment is not until mid-June. I can ask the pulmonologist at that time.
In the meantime, I learned today that the pulmonologist has now ordered a c-pap, which I pick up on Friday. I did do a sleep study and evidentally it showed that this device will help with my circumstances, so he says.
Regardless, and in the meantime, I would still like to know what's really going on. I'm so tired of the pain pills, the Lasix, the antibiotics, the tranquilizers, etc... This whole routine is getting me down and my quality of life has just almost all but bottomed-out. I really need some direction on this disorder. It's all just taking so long to find a diagnosis and remedy. Why? I just don't understand.
Thanks for taking time to respond.
.
No, I don't mind. Sorry I didn't mention the medications. Yes, I'm currently taking Lasix, and was also prescribed that while in the hospital, but things haven't changed much in a month. I swell up; I go to bed, the swelling goes down, I pee all day, the swelling comes back up and the cycle starts all over on a daily basis. Just some days are worse than others. :-(
Actually, I went to a Cardiologist BEFORE I went to the ER the first time in the first week of February, i.e. when I first started having an inkling of swelling in my feet & legs, because my first thoughts were that of heart failure. As a matter of fact, I saw him before they really ballooned up and turned red a week later. However, he never looked at my feet or legs much except to notate that, "Yes, they look "a little swollen", (looking through my socks, mind you... )
Beings that I have an echocardiogram that suggests mitral valve regurgitation, I wanted this re-checked as well. The last echo was about ten years ago. The only thing this current cardiologist really did for me was run a full blood count; in which all he found were normalities; and then he ran another echo which was found that I have 54% regurgitation which is increased from the original 46%, BUT, it is an oddity that he did not respond to the mmHg 84 pressure on my heart, which I'm told by several, including my current pulmonologist, that this is pretty high and that doctor was asking me why the Cardiologist did not act on this. I could only answer, "I don't know. I'm not the doctor".
The Cardiologist told me that he did not hear the usual "murmur" that is normally heard with mitral valve regurgitation or prolapse. I honestly don't know what that means to him. Why the cardiologist did nothing for me at that time, I simply have no clue at this juncture. I went to him because he was highly referred and is considered one of the best in the country. After the visit, he simply referred me to a pulmonologist and then back to my primary for treatment for the legs, which so far, has gone no where.
I have not heard of LVF. But, I'm assuming is probably "Left Ventricular Failure"? Or something like that? You would think with all the poking, sticking, scans, and bloodwork that's been done that CHF or LVF, as you've mentioned, would be looked upon as a possibility. My soonest next appointment is not until mid-June. I can ask the pulmonologist at that time.
In the meantime, I learned today that the pulmonologist has now ordered a c-pap, which I pick up on Friday. I did do a sleep study and evidentally it showed that this device will help with my circumstances, so he says.
Regardless, and in the meantime, I would still like to know what's really going on. I'm so tired of the pain pills, the Lasix, the antibiotics, the tranquilizers, etc... This whole routine is getting me down and my quality of life has just almost all but bottomed-out. I really need some direction on this disorder. It's all just taking so long to find a diagnosis and remedy. Why? I just don't understand.
Thanks for taking time to respond.
.
Loading...
hi, sorry for the delay in responding. Thanks for the extra info, i have seen evidence that links sleep apnoea with peripheral oedema, most commonly however in females over the age of 50, post-menopausal or overweight. i am glad to hear that you have been fitted for c-pap, this is a very effective treatment and although cumbersome to wear for some people, the benefits reported by those same patients far outweigh the cons!
If the peripheral oedema is related to the sleep apnoea then within time you will hopefully begin to notice a difference with using the c-pap, if not with the oedema then certainly with the other symptoms such as the dizziness, tiredness etc which will in turn aid your mobility and state of mind.
I really hope that things continue to improve for you, any further questions feel free to post again.... casig
If the peripheral oedema is related to the sleep apnoea then within time you will hopefully begin to notice a difference with using the c-pap, if not with the oedema then certainly with the other symptoms such as the dizziness, tiredness etc which will in turn aid your mobility and state of mind.
I really hope that things continue to improve for you, any further questions feel free to post again.... casig
Loading...
Have you been tested for M.S.? I have the same symtoms and was told it's because I set in a wheelchair.
Loading...
I am so glad I cam upon your posting. I too woke up with very painful red/ purple swollen feet. I have been given the turn around and I am being fitted for cpap machine as well as as oxygen. My feet hurt worse to elevate but like you said in your post the swelling goes down and after you get up on them after an hour or so the swelling comes back with and it seems like it gets to be more painful. I wish I could find out where you live and check to see what you have done ot accommodate your feet.
Thanks Brandon
Thanks Brandon
Loading...
Hi,
Sorry for the delay in response.
I've really had a struggle this past week with the c-pap. I've done things with that machine in my sleep that I don't know about until I've woke up. They told me to give it time. I tried laying and just watching TV with it on to see what it does after the ramp timer .. and it does push quite a lot of air thru and into your lungs. My rib cage ached for the first three days, but it doesn't hurt anymore.
No, I haven't been tested for MS. The doctors contribute my problem to COPD and Pulmonary Hypertension, I'm being told unofficially, this past Thursday. It still does not answer my questions about my legs tho. I must admit, however, the swelling is not as intense as it was. Perhaps the combination of oxygen and the cpap are working, along with the lasix.
I live in Oklahoma. If you'd like to write to me privately, please reference this website :::
*****
Thanks.
~ kat
**edited by moderator**
Sorry for the delay in response.
I've really had a struggle this past week with the c-pap. I've done things with that machine in my sleep that I don't know about until I've woke up. They told me to give it time. I tried laying and just watching TV with it on to see what it does after the ramp timer .. and it does push quite a lot of air thru and into your lungs. My rib cage ached for the first three days, but it doesn't hurt anymore.
No, I haven't been tested for MS. The doctors contribute my problem to COPD and Pulmonary Hypertension, I'm being told unofficially, this past Thursday. It still does not answer my questions about my legs tho. I must admit, however, the swelling is not as intense as it was. Perhaps the combination of oxygen and the cpap are working, along with the lasix.
I live in Oklahoma. If you'd like to write to me privately, please reference this website :::
*****
Thanks.
~ kat
**edited by moderator**
Loading...
hi, glad to hear you have been fitted with the cpap, although difficult as i said before it will be worth it in the end. It may be that your equipment will require "tweaking" to suit you and your condition but that will all be worked out during folow up appointments. As i said before if the swelling is related to the sleep apnoea ( inc pulmonary hypertension ) the you should hopefully notice a significant improvement shortly.. the best of luck with your condition... casig
Loading...
Hi,
I'm back to report that I've been hospitalized again. This time with pneumonia, exacerbated by the c-pap and have subsequently been removed from the machine.
There has been a discovery of exceptionally large lymph nodes in my medialstinum vicinity. CT Scans and PET Scans show normal appearances with no cancer.
The doctor wants to do a brush-by biopsy to see what is encapsulated in my medialstinum. His initial diagnosis is that this may be sarcoidosis. However, as he stated, I do not fit the protocol for this condition, i.e. young afro-american females are usually who present this problem. I am over 50 white caucasian. So chances of this being sarcoidosis is probably fairly slim to none.
MY PERSONAL diagnosis is Castleman's Disease. However, Castleman's is usually found in the paravertebral superior mediastinum, not in the medialstinum vicinity. BUT, I do believe it's a clear possibility.
>>>>
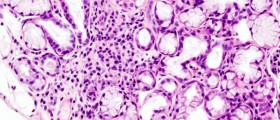
Giant Lymph Node Hyperplasia of the Mediastinum (Castleman's Disease):
Case Report and Review Muhammad A.K. Bhatti, M.D., M.B.B.S., John W. Ferrante, M.D., Isaac Gielchinsky, M.D., and John C. Norman, M.D. Department of Surgery, Muhlenberg Hospital, Plainfield, New Jersey Department of Thoracic and Cardiovascular Surgery, Newark Beth Israel Medical Center, Newark, New Jersey.
Giant lymph node hyperplasia is a rare, benign disease involving lymph nodes in various locations, predominantly in the mediastinum. There are two variants: plasma cell (earlier and/or acute) and hyaline-vascular, more chronic with an intermediate transitional type. The usual presentation is a solitary well-circumscribed asymptomatic mass lesion, often attaining large size, with infrequent associated hematologic manifestations. A case of giant lymph node hyperplasia involving the paravertebral superior mediastinum is reported.
Surgical excision was the treatment of choice in a 65-year-old man, and at thoractomy, an encapsulated mass was excised from the posterior superior mediastinum. The patient had an uneventful postoperative course and was discharged on the tenth postoperative day.
Three years later, he is well and employed as a carpenter.
<<<
What does this have to do with my legs you may ask??? Well, obviously there is a kind of phoresis involved here. Unfortunately edema sets in a variety of places and for whatever reasons, it has settled in my legs, although the problem is of a pulmonary basis. STRANGE... but true.
So, I will continue to follow-up with my doctors, who are still scratching their heads... by the way. Hopefully, they will come up with something more concrete in the near future, and I can be getting back to some kind of normalcy in my life.
Right now, my quality of life is pretty nil. I can't work. I can't do much around my home. It is basically a sit and wait thing with me. So... what can I do???
I just know I'm very tired of all of this.
~ kat
I'm back to report that I've been hospitalized again. This time with pneumonia, exacerbated by the c-pap and have subsequently been removed from the machine.
There has been a discovery of exceptionally large lymph nodes in my medialstinum vicinity. CT Scans and PET Scans show normal appearances with no cancer.
The doctor wants to do a brush-by biopsy to see what is encapsulated in my medialstinum. His initial diagnosis is that this may be sarcoidosis. However, as he stated, I do not fit the protocol for this condition, i.e. young afro-american females are usually who present this problem. I am over 50 white caucasian. So chances of this being sarcoidosis is probably fairly slim to none.
MY PERSONAL diagnosis is Castleman's Disease. However, Castleman's is usually found in the paravertebral superior mediastinum, not in the medialstinum vicinity. BUT, I do believe it's a clear possibility.
>>>>
Giant Lymph Node Hyperplasia of the Mediastinum (Castleman's Disease):
Case Report and Review Muhammad A.K. Bhatti, M.D., M.B.B.S., John W. Ferrante, M.D., Isaac Gielchinsky, M.D., and John C. Norman, M.D. Department of Surgery, Muhlenberg Hospital, Plainfield, New Jersey Department of Thoracic and Cardiovascular Surgery, Newark Beth Israel Medical Center, Newark, New Jersey.
Giant lymph node hyperplasia is a rare, benign disease involving lymph nodes in various locations, predominantly in the mediastinum. There are two variants: plasma cell (earlier and/or acute) and hyaline-vascular, more chronic with an intermediate transitional type. The usual presentation is a solitary well-circumscribed asymptomatic mass lesion, often attaining large size, with infrequent associated hematologic manifestations. A case of giant lymph node hyperplasia involving the paravertebral superior mediastinum is reported.
Surgical excision was the treatment of choice in a 65-year-old man, and at thoractomy, an encapsulated mass was excised from the posterior superior mediastinum. The patient had an uneventful postoperative course and was discharged on the tenth postoperative day.
Three years later, he is well and employed as a carpenter.
<<<
What does this have to do with my legs you may ask??? Well, obviously there is a kind of phoresis involved here. Unfortunately edema sets in a variety of places and for whatever reasons, it has settled in my legs, although the problem is of a pulmonary basis. STRANGE... but true.
So, I will continue to follow-up with my doctors, who are still scratching their heads... by the way. Hopefully, they will come up with something more concrete in the near future, and I can be getting back to some kind of normalcy in my life.
Right now, my quality of life is pretty nil. I can't work. I can't do much around my home. It is basically a sit and wait thing with me. So... what can I do???
I just know I'm very tired of all of this.
~ kat
Loading...
My mother is suffering from the same symptoms. Her legs and feet swell up 4-5 times their normal size and turn purple. I was worried she was getting gangrene. She was also diagnosed with cellulitis along with many other things. She's at Mayo in Phoenix now trying to get help. If you get any answers please let me know.
Loading...
Starting about 6 inches below my knees my legs are swollen down to my toes. My legs are red, warm almost blistered. My legs in that area are so sore and tender down to the bone I cant touch them. Two days ago I woke up and the were bright bright red. Burnt, and extremeley painful.
I would be very interested if anyone finds out what this is.
I would be very interested if anyone finds out what this is.
Loading...
My mother has been going through the exact same thing. If you find out anything please post!
Loading...
I won't cover everything my husband has had and gone through, but all of your symptoms have been his at one time. He was diagnosed with RA and also Wegener's Vasculitis; now has severely damaged lungs and pulmonary hypertension and is on Flolan. But what caused all of this I believe is that 10 years ago at the beginning of all this he somehow contracted MRSA. He's had it 2 more times since then and it may be that they it never really went away. It is just recently that doctors know anything about this or have even tested for it and sometimes it still doesn't show up. They finally found it in a sputum test. It all started in his feet. First they went numb, then they hurt, then he had terrible red spots that developed in open wounds, and then it hit his lungs, then kidneys, but again, it took them almost 10 years to discover what was causing everything and by then, his lungs were about gone. Unfortuntely, before it was diagnosed, he had gone through chemo treatments 3 times and been put on various other antibiotics that only worked temporarily.
All I can say is please ask the doctors to check for NRSA before it's too late, although sometimes it can't be stopped.
All I can say is please ask the doctors to check for NRSA before it's too late, although sometimes it can't be stopped.
Loading...
I'm on no medication, and the swelling as been going on for 3 months. I'm starting to get a tad bit worried. I'm a wrecker driver. So, I'm not on me feet that much. This sleep thing "apnoea" not sure what the is, but I have all kinds of sleep problems. maybe thats related, and I'm sure my weight doesn't help. But three months? I don't want to go to a doctor but maybe I should.
Loading...
I think cellulitis is a convienant catch-all disease/word. I have been anorexic since my teens and took diuretics off and on to lose weight. One day my feet swelled up and turned red/purple and my family doctor sent me to the hospital, where they said it was cellulitis. I was 26. I am 50 now and they still swell up and down. At the end of the day they are huge and in the morning they are better. I also have chronic kidney disease and will soon start dialysis or have to have a transplant. I have 15% kidney function in one kidney and none in the other. My family doctor says it is because of my kidneys (swelling feet) and my kidney doctor says some of it can be attributed to kidney function but it's not caused by that. I have also been told it is due to electrolyte imbalance- decreased potassium. Anyway, everyone thinks my feet look wierd -especially me. They are most painful on the bottom tho'- they are very hard and sort of knobby on the bottom, even when they are not swollen. And now I have to take diuretics.
Loading...