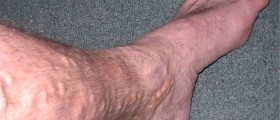
The blood vessels you see in your legs and feet are part of the venous network of vessels that pump blood to the heart through a series of valves with the help of the leg muscles. The valves in the walls of the veins serve to ensure a one-way flow of blood towards the heart, while the muscles of the legs promote the pumping of the blood to the circulation during ambulation. At rest, when the muscles are not contracting, blood may pool in the legs and feet if the valves are not working properly (incompetent valves). This leads to chronic venous insufficiency, a problem where there is inadequate flow of blood from the leg veins of the legs back to the heart. It is also called chronic venous stasis because blood tends to flow backward and pool in the legs, leading to problems such as varicose veins.
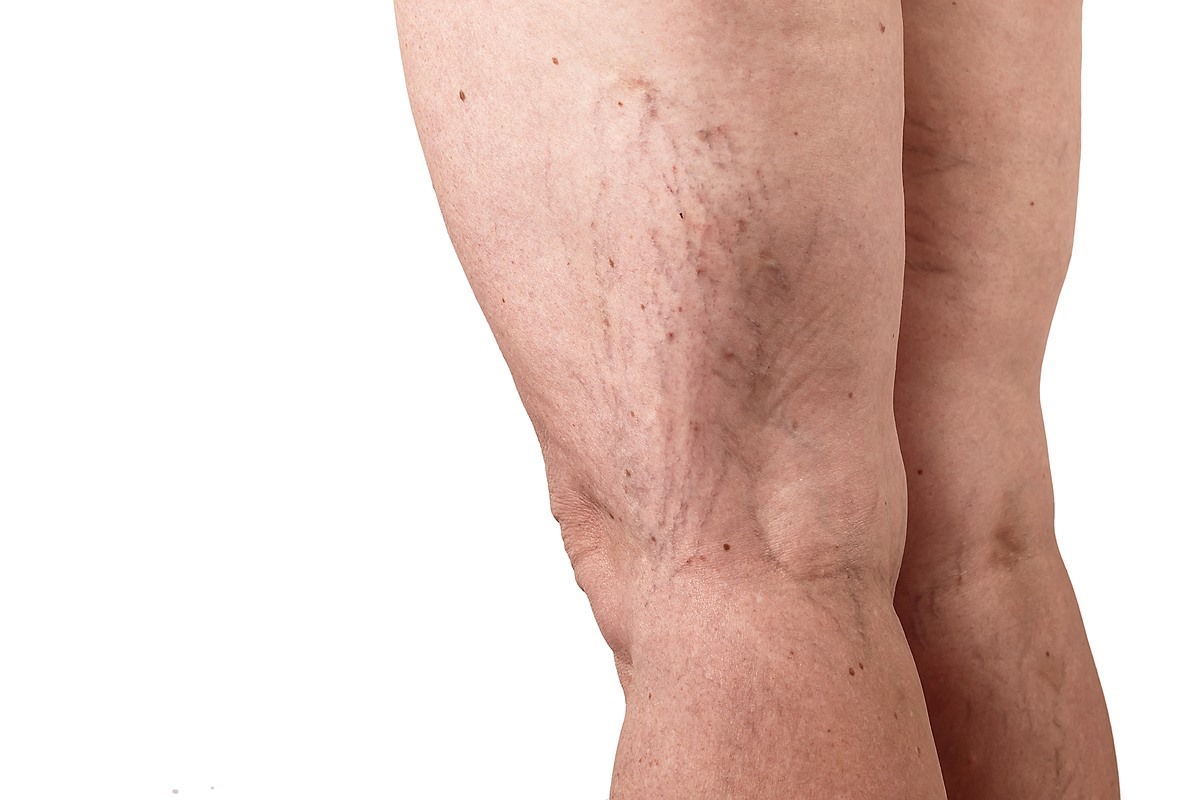
Symptoms of chronic venous stasis include:
- Swelling of the ankles
- Itching
- Throbbing pain
- Cramping
- Leg aches
- Leg fatigue
- Tight feeling in the calves
- Feeling of heaviness in the legs
- Non-healing skin sores or ulcers
- Pain when walking, relieved with rest
- Changes in skin color, especially near the ankles
- Capillary proliferation, or increase in small blood vessels
Causes
Chronic venous insufficiency is a common medical problem that affects up to five percent of the American population. It is sometimes caused by formation of blood clots (deep vein thrombosis) and increased blood pressure inside the leg veins. It is more common among females, obese, pregnant, and elderly individuals. Other factors that increase your likelihood of developing chronic venous insufficiency include:
- Having a family history of the condition.
- Leg injury, surgery, or history of previous blood clots
- Prolonged sitting or standing
- Smoking
- Lack of exercise
- Swelling and inflammation of a leg vein (phlebitis)
Treatment
Home remedies to reduce symptoms of chronic venous stasis include:
- Use of compression stockings to reduce swelling and pain.
- Getting more exercise, such as walking increase blood flow.
- Keeping the legs raised above the level of the heart when lying down to reduce swelling.
- Avoiding standing or sitting for long periods to reduce pooling of fluids in your legs.
- Avoiding a crossed-leg position.
Medical treatments may include:
- Medications such as diuretics (water pills) may be prescribed when you have other conditions that may be contributing to the swelling (such as heart disease or kidney disease). Other medications that improve blood flow of blood through the veins may be used in addition to compression therapy.
- Sclerotherapy, which involves injecting a chemical into affected veins. This causes the veins to scar and close, thus diverting blood flow through other veins.
- Surgery, which may be recommended for some patients include:
- Ligation and "vein stripping," a procedure that involves tying off a vein and removing damaged veins.
- Surgical repair of veins.
- Vein transplant, which involves replacing a diseased vein with a healthy vein.
- Subfascial endoscopic perforator surgery, which involves the use of a small, flexible tube with a camera lens to clip and tie off damaged veins.
- Johns Hopkins. Chronic Venous Insufficiency. http://www.hopkinsmedicine.org/healthlibrary/conditions/cardiovascular_diseases/chronic_venous_insufficiency_85,P08250/
- WebMD. Venous Insufficiency. http://www.webmd.com/a-to-z-guides/venous-insufficiency-topic-overview
- Medscape. Venous Insufficiency. http://emedicine.medscape.com/article/1085412-overview
- Photo courtesy of SteadyHealth