Table of Contents
Classified as an autoimmune condition, reactive arthritis develops in response to an infection in another part of the body, almost exclusively either in the genitals or bowel. The most common triggering infection is Chlamydia, although Shingles and Salmonella are also known to provoke the condition as well. Complaints include joint pain and swelling, particularly in the knees, ankles and feet, however the eyes, skin and urethra may also be inflamed.
Reactive Arthritis: Mechanism Of Disease
Reactive arthritis presents itself in the patient about one to three weeks after the initial infection. Exactly how and why the patient’s immune system reacts to the infecting bacteria in this way is unknown. After extensive research, scientists have concluded that the condition is caused either by bacterial antigens that, for some reason, have been deposited in the joints, or by an autoimmune response involving cross-reactivity of bacterial antigens with tissues in the joints.
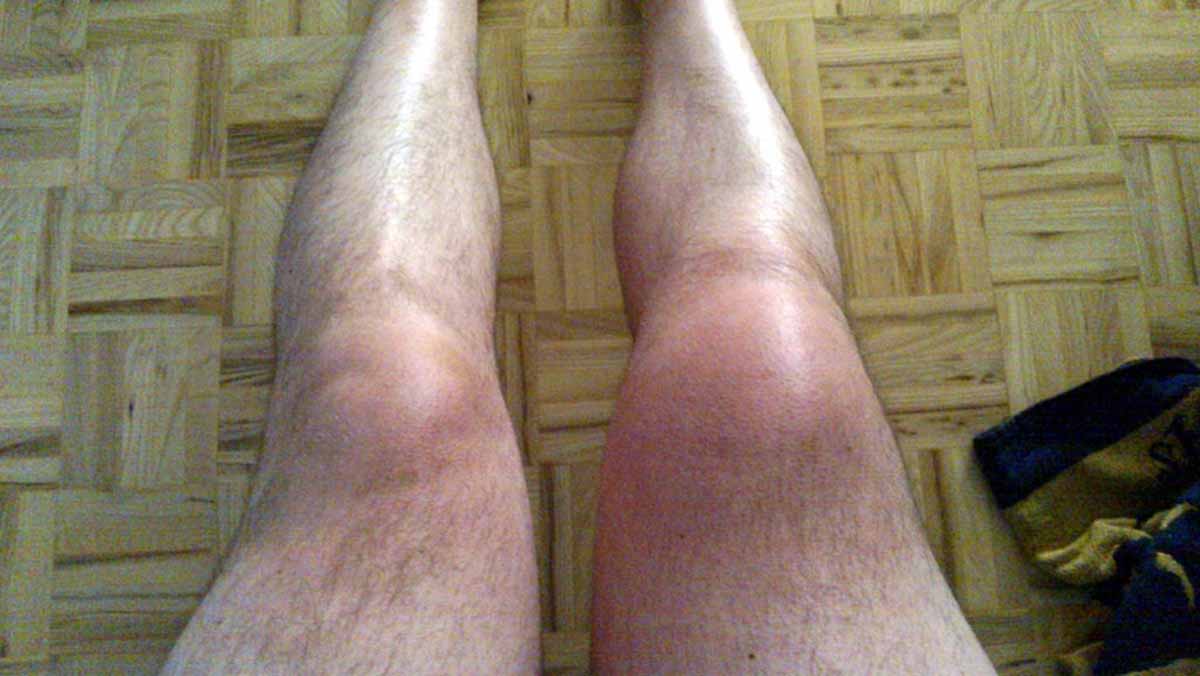
The human body responds to an infection by generating antibodies and other chemicals to attack and eradicate the infecting germ. Various debris and other chemicals can be the by-product of this attacking process, and it is this debris that may become lodged and stuck in the joints, triggering inflammation and ultimately, reactive arthritis.
Risk Factors And Genetic Predisposition
The clinical pattern of reactive arthritis consists of fewer than five joints presenting with inflammation. The condition may progress logically whereby more joints become inflamed in addition to the initially infected site, or it may appear to improve but new joints then subsequently become inflamed. Individuals aged between 20 and 40 years of age are at most risk, and in general, men are affected more than women. This is particularly true in the case of instances linked to sexually transmitted diseases. In addition, a genetic link has also been found. White people are around 50 times more likely to develop reactive arthritis owing to the high frequency of the HLA-B27 gene in the white population. In the UK, 1 in 14 people have this gene, which seems to make them much more likely to develop reactive arthritis in response to a triggering infection.
Antibiotics And Anti-Inflammatory Drugs To Relieve Symptoms
So what can be done about it? At present, there is no known cure for reactive arthritis. Instead, treatment is centered around relieving the symptoms based on their severity. In the majority of cases, symptomatic treatment and supportive care are all that is needed to see the patient through to complete recovery. These include oral antibiotics to combat the initial infection and non-steroidal anti-inflammatory drugs, known as NSAIDs, to treat inflammation and pain in the joints. Long term use of NSAIDs is not usually recommended though, as they can lead to stomach ulcers and other digestive issues.
- Keat A et al, 1987, Chlamydia trachomatis and reactive arthritis: the missing link. The Lancet, 329(8524), 72-74
- Toivanen P and Toivanen A, 1999, Two Forms Of Reactive Arthritis? Annals of the Rheumatic Diseases, 58, 737-741
- Hermann E et al, 1993, HLA-B27-restricted CD8 T cells derived from synovial fluids of patients with reactive arthritis and ankylosing spondylitis. The Lancet, 342(8872), 646-650
- Carter JD et al, 2010, Combination antibiotics as a treatment for chronic Chlamydia-induced reactive arthritis: a double-blind, placebo-controlled, prospective trial. Arthritis and Rheumatism, 62(5), 1298-1307
- Tanaka T et al, 2009, Successful treatment of reactive arthritis with a humanized anti-interleukin-6 receptor antibody, tocilizumab. Arthritis Care & Research, 61(12), 1762-1764.
- Photo courtesy of ::Tanty:: via Flickr: www.flickr.com/photos/tanty0/16595983943
- Photo courtesy of Joe Shlabotnik via Flickr: www.flickr.com/photos/joeshlabotnik/419914250


Your thoughts on this