Due to early detection methods, increased sun exposure and an aging population, rates of skin cancer increase annually.
What is Skin?
In order to understand the differences between basal and squamous cell cancers, it is necessary to know about the function and structure of skin. Skin is the largest organ of the body and functions in several different ways:
- Protects and covers the internal organs of the body
- Acts as a barrier to germs such as bacteria
- Prevents the loss of fluids and water in the body
- Helps in regulation of body temperature
The skin has three layers, the dermis, epidermis and subcutaneous. The epidermis is the top layer of skin, which protects the underlying layers of tissue and organs from elements of the environment. The middle layer of skin is called the dermis, which is considerably thicker than the epidermis.
The dermis contains the sweat glands, hair follicles, blood vessels and nerves which are held in place with collagen (an insoluble fibrous protein). The subcutaneous or subcutis layer is the final and deepest layer of the skin,which conserves heat and protects internal organs from injury.
Different Types of Skin Cancer
Melanomas are skin cancers that begin from melanocytes, which are the cells that make pigmentation (responsible for skin color). Melanocytes can also cause benign skin growths called moles. Non-melanoma skin cancers are groups of cells that are not cancerous, these types of growths tend to act in a manner completely different than melanomas.
Keratinocyte carcinomas or keratinocyte cancers are the second main type of skin cancer. When examined under a microscope these cancers share some of the same features as keratinocytes, the most common cell type found in normal skin. Basal cell carcinomas and squamous cell carcinomas are the most commonly diagnosed forms of keratinocyte cancers.
When basal cell carcinomas are viewed under a microscope these types of cancer share characteristics with cells in the lower layer of the epidermis. Between 1 and 8 cases of skin cancers are basal cell carcinomas, which usually develop on the ears, neck and head, and usually found in middle aged and older people.
Because basal cell carcinomas are slow growing, it is rare for cancer of this type to spread to nearby lymph nodes or other parts of the body. If left untreated however, the cancer can grow into nearby areas and invade bone and other tissues underneath the skin. Once treated, basal cell carcinomas can return in the same spot on the skin and as many as half of all people diagnosed will experience a recurrence within 5 years.
Squamous cell carcinomas account for approximately 2 out of 10 cases of skin cancer and commonly occur on the face, lips, neck, ears and the back of the hands. Oftentimes cancer of this type start in actinic keratosis (a pre-malignant condition) and sometimes form in the genital area. Squamous cell cancer is more aggressive than basal cell, and is more likely to invade adipose tissue located under the skin and spread to the lymph nodes or distal areas.
Keratoacanthomas are cancerous growths found in areas of the skin that experience a high level of sun-exposure. Many keraoacanthomas will shrink or go away spontaneously and do not require treatment, but some continue to grow and may spread to other parts of the body. The growth of a keroacanthoma is hard to predict and many dermatologists and skin specialists believe it is better to consider them as a form of squamous cell skin cancer.
Less Common Forms of Skin Cancer
Melanomas and keroacanthomas are two of the most common forms of skin cancer, however, there are also some less common forms as well. These types of cancers are referred to as “non-melanoma skin cancers,” and are quite different from keratinocyte cancers and require different treatments. Types of non-melanoma skin cancer include the following:
- Merkel cell carcinoma
- Cutaneous skin lymphoma
- Kaposi sarcoma
- Skin adnexal tumors
- Several types of sarcomas
When all of these types of cancer are combined, they account for less than 1% of all non-melanoma skin cancers diagnosed.
Merkel cell carcinoma is a rare type of skin cancer that develops in the neuroendocrine (hormone-making cells) cells of the skin. Merkle cell carcinomas are thought to be caused by sun exposure and can start anywhere but are found primarily on the head, neck and arms. Cancers of this type often return after being treated and may spread to the lymph nodes and other internal organs, which is not common of squamous cell carcinomas or basal cell carcinomas.
Prior to the 1980's, Kaposi sarcoma was rare and mostly presented in elderly people of Mediterranean descent. Kaposi sarcoma typically begins within the dermis, but can also be found within internal organs as well. This type of cancer has become more common because it is prevalent in people with acquired immunodeficiency syndrome (AIDS) and human immunodeficiency virus (HIV).
Skin lymphomas are cancers that begin in the lymphocytes which are a type of immune system cells located in the bone marrow (soft, spongy inner part in some types of bones), lymph nodes (bean-sized cells of the immune systems), bloodstream and internal organs.
Though most lymphomas begin within the lymph nodes or internal organs, there are certain types that may appear to begin within the skin. The most prevalent type of primary cutaneous lymphoma diagnosed is cutaneous T-cell lymphoma (called mycosis fungoides).
Adnexal tumors begin in the hair follicles or glands of the skin. While it is very rare for tumors of this type to be malignant, benign tumors of this nature are common.
Sarcomas develop in the connective tissue cells, usually located deeply under the skin. Less commonly sarcomas develop in the dermis and subcutaneous layer of the skin. There are many types of sarcomas that develop in the skin such as dermatofibrosarcoma protuberans and angiosarcoma (blood vessel cancer).
Most tumors found on the skin are benign and rarely develop into cancer. Tumors of this nature include the following:
- Moles (most types)
- Hemangiomas: benign blood vessels, often referred to as strawberry marks, port wine stains and stork bites
- Lipomas: soft growth of benign fatty cells
- Sebhorrheic keratoses: brown, tan or black raised spots with a rough surface or waxy-like appearance
- Warts: roughly surfaced growths that are caused by a virus
Precancerous or pre-invasive skin conditions may develop into skin cancer or might possibly be early stage skin cancer. Some forms include the following:
Actinic keratosis: a precancerous skin condition also known as solar keratosis, caused by direct overexposure to sunlight. These are small rough spots that are generally pinkish-red or flesh colored and usually develop on the ears, face, arms and back of hands. Usually occurring in the elderly population and people with fair skin, though it can happen on any other area of the body that receives excessive sunlight exposure.
Squamous cell carcinoma in situ (Bowen disease): the condition is the earliest form of squamous cell carcinoma, in situ denotes that these types of cancer cells are still located entirely within the epidermal layer and have not spread to the dermis. Appearing as reddish patches, Bowen disease patches are larger when compared with actinic keratoses. This form is less invasive than other types of skin cancers, and Bowen disease of the anus and genital skin are more than likely due to the human papilloma virus (HPV).
What are the Risk Factors Associated with Skin Cancer?
Risk factors are things that affect a persons chance of developing a disease, such as cancer. Different types of cancers have different risk factors, but having an increased risk does not mean a person will definitely develop cancer. The following list contains known risk factors of basal cell carcinomas, squamous cell carcinomas, (but list does not apply to other forms of non-melanoma skin cancer such as cutaneous lymphoma and Kaposi sarcoma):
Ultraviolet (UV) light exposure: believed to be the biggest risk factor associated with skin cancer. Exposure to direct sunlight is the most common form of UV radiation, other sources include sun lamps and tanning booths, overexposure can lead to damage in the genes of skin cells. Sun overexposure in youth is one of the many things that raises the chance of developing skin cancer.
Being fair skinned: the risk factors for skin cancer are higher for people of Caucasian ethnicity than for African Americans of Latinos. Due to the protective effect of melanin (skin pigmentation), Caucasians with fair (lightly colored) skin tones that freckle or burn easily, are at an increased risk. This accounts for the higher rates of skin cancer in Australia and the British Isles. People with congenital (present from birth) albinism have no skin pigment, pink-white skin and white hair. Because of the lack of melanin and a high risk for skin cancers, albinos must be extremely careful to protect skin from UV rays.
Older age: as people age, the risk of squamous cell carcinoma increases, maybe in part because of the accumulation of sun overexposure throughout a lifetime. However, cancers of this type are now showing up in the younger population, which is likely due to spending more time in the sun and not having adequate protection or using sunscreen.
Males: men are twice as likely as a female to develop basal cell cancers, and three times more likely to have squamous cell cancers, the cause is thought to be linked to higher levels of sunlight exposure.
Being exposed to certain chemicals: being exposed to large amounts of arsenic is directly linked to an increased risk of skin cancer. Arsenic is a metal found naturally in well water, and is also used in making some types of pesticides and medications. People who work around coal, tar, paraffin and certain types of oils may also have a higher risk of non-melanoma skin cancer.
Exposure to radiation: people who have had radiation treatment have a higher likelihood of developing skin cancer in the same area that was treated. Children who have received radiation treatment have particular problems due to this fact. Most types of cancers that evolve from radiation exposure are basal cell carcinomas.
Past history of skin cancer: people who have had a previous diagnosis of skin cancer have a much higher chance of recurrence.
Long-term severe skin inflammation or injury: though the risk is small, people with scars from burns or areas of skin over severe bone infections and skin damage from chronic inflammation, are more likely to develop keratinocyte skin cancers.
Psoriasis treatment: psoralen and UV treatment are two common treatment protocols for psoriasis (chronic inflammatory skin disorder), people who have had these treatments are more likely to have squamous cell skin cancer and other forms as well.
Xeroderma pigmentosum (XP): a very rare condition that is inherited, reduces the ability of the skin to repair damaged deoxyribonucleic acid (DNA). People who have XP often develop skin cancers, which sometimes beginning in childhood.
Basal cell nevus syndrome: rare, congenital (present at birth) condition that causes multiple skin cancers. Most cases of this disorder are inherited, people affected often have jaw, bone, eyes and nervous tissue abnormalities.
Compromised immune system: the immune system helps the body fight off infections, illness and cancer of the skin and other organs. People who have a compromised immune system (due to certain diseases such as HIV, or medical treatment such as an organ transplant), are more prone to developing non-melanoma skin cancer.
Human papilloma virus (HPV) infection: human papilloma virus is a group of more than 100 different viruses that can cause papillomas (warts). Certain types of HPV can result in genital and anal warts, which are related to skin cancer occurring in these areas.
Smoking: people who smoke are more prone to squamous cell skin cancer, particularly on the lips.
Genetic susceptibility: researchers have found that certain groups of people are more likely to develop skin cancer than others, in this type of person the chromosomes are predisposed to sunlight damage.
What Causes Skin Cancer?
Unprotected UV radiation exposure is the cause of most basal cell and squamous cell skin cancers. Overexposure may have occurred years before the development of skin cancer, but repeated unprotected exposure to the sun over a long period of time increases the risk. UV radiation damages DNA, sometimes the damage can affect certain genes (DNA segments with a specific function) that control cell growth and function.
In most cases, the body can repair DNA damage due to overexposure, however, if there has been too much, in some cases skin cancer can result. Researchers do not know how all of the DNA changes can lead to skin cancer, but it is known that many forms of skin cancer contain changes in tumor suppressor genes, which normally keep cells from growing to rapidly.
The most common gene found to mutate in basal cell skin cancers is the “patched” gene. This tumor suppressor gene normally regulates cell growth, however changes to this particular gene can result in out of control cell growth. These changes in tumor suppressor genes play a critical role in the development of skin cancer, along with many others.
Scientists are currently researching links between DNA changes and skin cancer. In the future, a better understanding of how damaged DNA is linked to skin cancer could be useful when trying to find treatments to overcome or repair cell damage.
Can Skin Cancer be Prevented?
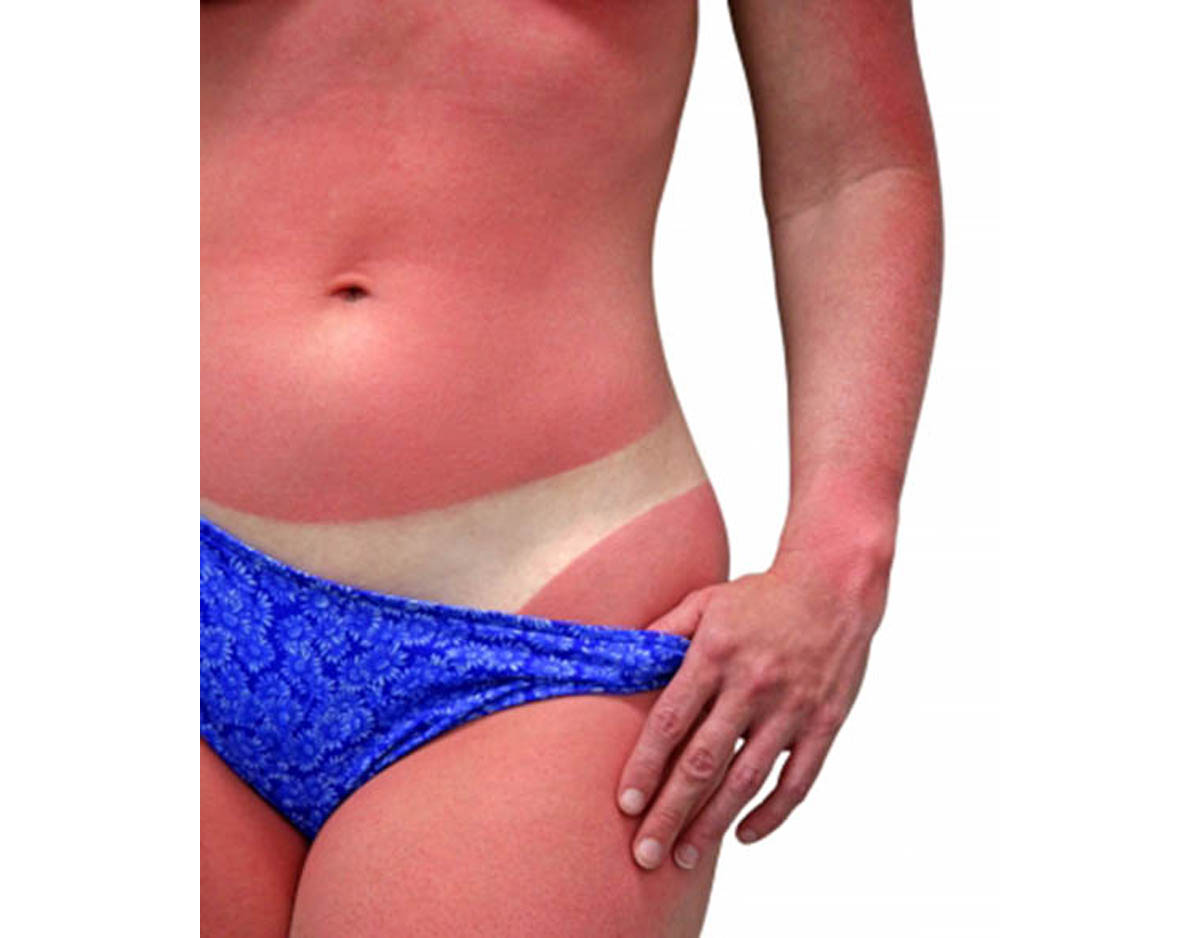
While not all forms of skin cancer can be prevented, there are ways a person can reduce certain risk factors. The following information includes ways to limit the risk of skin cancer:
Limit ultraviolet exposure: one of the most important ways a person can reduce the risk of basal and squamous cell skin cancer is to limit exposure to UV rays. Practice sun safety, wear protective eye wear, use sunscreen regularly, put on a shirt and over sized hat anytime skin is exposed to direct sunlight.
Wear protective clothing: clothing offers different levels of protection from sun exposure. Long-sleeved shirts, long pants and long skirts offer a person the most protection and darker colors generally provide better protection than lighter colored clothing. Some clothing manufacturers in the U.S. are now making clothes that are lightweight and offer UV protection, even when wet. The higher the level of a sunscreen, the more protection is offered against UV rays.
Regular use of sunscreen: the American Cancer Society recommends regular use of sunscreen as part of a UV protection regimen. Using sunscreens and lip balms with an SPF (sun protection factor) of 15 or higher is especially important when being exposed to sunlight for long periods of time, in a hot environment or high altitude, and during peak sunshine hours (10 am-4 pm).
Wrap around sun glasses: up to 99% of rays can be absorbed by wearing wrap-around sunglasses. When shopping for sun glasses, search for brands that block UVA and UVB rays, verify if the label states “meets ANSI UV requirements,” if there is no label, the sunglasses may not provide adequate protection.
Stay in the shade: limit UV exposure by seeking shaded areas when outdoors during prime sunlight hours from 10 am until 4 pm. If a person is unsure of how intense the sun rays are, doing the shadow test is necessary: if the shadow is shorter than a person, the sun rays are strong and the person should seek out shade.
UV index: the amount of UV rays that reach the ground, depends upon a number of factors; the time of day and year, elevation and cloud cover. The National Weather Service and the United States Environmental Protection Agency (EPA) have developed the UV index which helps people better understand the intensity of UV rays. If the number of the UV index is higher it means there is an increased chance of sunburn, skin damage and development of skin cancers of all types.
Avoid other types of UV light: using tanning beds or sunlamps is dangerous because the UV radiation delivered, can cause skin damage. Mounting evidence suggests prolonged use raises the chances of getting skin cancer, most physicians recommend people avoid tanning beds and sun lamps completely.
Protecting children from the sun: small children require extra attention because they spend more time outside and can become sunburned easier. Parents and childcare providers should protect children from long periods of sun exposure and always observe a sun protection program. Use of hats, sunscreen and protective eye wear is always recommended and avoiding direct exposure during the peak hours (10 am until 4 pm) should be observed.
Sun exposure and vitamin D: vitamin D has many healthful benefits, and can lower the risks of some types of cancer. Vitamin D is naturally manufactured by the body when the skin is exposed to sunlight. The amount of vitamin D the skin manufactures depends upon age, skin color and intensity of the sun light. For children that live in an area of very little sunlight or have darker skin tone, a vitamin D supplement may be necessary.
Avoid dangerous chemicals: exposure to certain harmful chemicals such as arsenic, can increase the risk of skin cancer. People can be exposed to arsenic in well water, pesticides, herbicides, some types of medications, herbal medications and in an occupational capacity. High levels of arsenic should be avoided.
Become educated about skin cancer prevention: several organizations conduct skin cancer workshops and prevention activities in schools, parks and recreational areas. There are brochures and public service announcements designed to educate people about the necessity of skin cancer prevention.
Can Skin Cancer be Detected Early?
Many types of cancers can be detected early and as a part of a routine cancer check up, a physician should do a thorough check of the skin and pay particular attention to moles and other skin abnormalities. It is also important that a person do regular checks of skin and moles, blemishes, freckles and other marks, a self-exam should be done in a well lit area in front of a full-length mirror and a hand held mirror should be used for hard to see areas.
Examination of all areas including the palms of hands and soles of the feet, scalp, ears, fingernails and toenails and back is necessary. Having a friend or family member to assist with the hard to see areas is a good idea as well.
The appearance of skin cancer can look like a variety of other marks on the skin, this is why it is so important to do a complete check over all areas of the body. New growths, spots that are growing larger or changing and sores that do not heal are all warning signs of skin cancer and should not be ignored.
How is Skin Cancer Diagnosed?
If an abnormal area of skin has the possibility of being skin cancer, there are a number of medical examinations and testing that can be done in order to make a definitive diagnosis. If there is a likelihood of the skin cancer spreading to other parts of the body, further tests may be conducted.
Skin cancer symptoms rarely become an issue until the cancer grows larger, at this point bleeding and pain are possible.
Basal cell carcinomas often appear as firm, flat, pale areas with a raised profile, and the area may bleed after being injured. Basal cell cancers have one or more visible abnormal blood vessels that have a depressed center, blue, black or brown areas and larger basal cell cancers could have an oozing or crusty surface.
Squamous cell carcinomas appear as growing lumps or bumps, have a smooth surface or may be slow growing, flat reddish-pink patches on the surface of the skin.
Both types of these non-melanoma skin cancer can develop as a flat area exhibiting on flight changes in appearance from normal skin.
There are other types of skin cancer than melanoma, basal cell carcinoma and squamous cell carcinoma, which include the following:
- Kaposi syndrome: usually begins as a small bruised-like area that could later develops into tumors.
- Mycosis fungoides: (form of lymphoma that begins in the skin) usually starts as a rash, often on the buttocks, lower abdomen and skin. Can appear similar to skin allergies and other forms of skin irritation.
- Adnexal tumors: look like bumps within the skin.
- Skin sarcomas: look like large masses beneath the surface of the skin.
- Merkel cell tumors: usually appear as firm, pink, reddish or purple nodules (hard, round, spherical abnormal structure) or ulcers (abrasions) on the face, legs or arms.
If the physician thinks a person has skin cancer, one or more of the following things will be done to confirm a diagnosis:
History and physical: a physician will take a medical history including age, note when the marks on the skin first became known, changes in size or shape of the marks, past exposure to known causes of skin cancer and if there is a family history of skin cancer. The physician will make note of the size, shape, color and texture and if there is bleeding or scaling of the spots on the skin. The entire body will be evaluated to check for marks or moles, the lymph nodes will be examined, if necessary the physician could make a referral to a dermatologist for further consultation.
Skin biopsy: if the physician suspects a mark on the body could be skin cancer, a sample will be taken from the area and sent to be examined under a microscope. Depending upon the size of the mark, location and suspected type of cancer, several different methods of skin biopsy could be used.
Lymph node biopsy: if the physician feels lymph node enlargement or firmness, a lymph node biopsy may be performed to determine if the skin cancer has spread.
How is Skin Cancer Staged?
Staging is the method used to find out how widespread a cancer may be. Basal cell cancer rarely spreads to other organs or locations in the body, so staging is seldom done unless the area of cancer is quite large. Squamous cell cancers have a higher risk of spreading so staging is sometimes done, especially in those who have a higher risk of spreading.
The American Joint Commission on Cancer's, TNM system is used to determine what stage of cancer development is present in the body. Physical examinations and testing are used to assign the T, N and M status and a group stage of cancer. The TNM system for staging of cancer stands for 3 key pieces of information; T stands for tumor, N represents the spread to nearby lymph nodes and M denotes metastasis (spreading to distant internal organ).
How is Skin Cancer Treated?
The treatments described below apply to actinic cancer, squamous cell carcinoma, basal cell carcinoma, Merkel cell carcinoma, lymphomas, Kaposi syndrome and other sarcomas:
Surgery: most forms of basal cell and squamous cell carcinomas are easily treated by minor surgery and the application of medications to the surface of skin. For certain types of skin cancer that have a higher likelihood of spreading, surgery will be followed up by either radiation or chemotherapy.
Forms of local therapy: several types of techniques can be used to treat skin cancer that has not metastasized to the lymph nodes or other locations in the body. Some of these methods are considered “surgery,” because they can destroy a targeted body tissue area. However, these techniques do not involve the use of scalpels or cutting of the skin.
Radiation therapy: the use of energy rays and particles (protons, photons or electrons) to kill off cancer cells. Radiation treatment focuses on the outside of the body and is the primary treatment next to surgery for treating skin cancer. Radiation can also be used in conjunction with other therapies, and can be used as adjuvant therapy after surgery to kill off any small cancer deposits that remain.
Systemic Chemotherapy (“chemo”): the use of anti-cancer medications injected into a vein or administered orally. The medication travels through the bloodstream to all locations in the body. Systemic chemo can attack cancer cells that have spread into lymph nodes and other areas. Side effects of chemotherapy include; hair loss, weight loss, mouth sores, poor appetite, fatigue, nausea and vomiting, lowered infection resistance and easy bleeding and bruising.
The side effects associated with chemotherapy will subside once treatment is concluded.
Clinical trials: carefully controlled research studies done with actual cancer patients. The studies are conducted to see whether a new treatment method is safe and effective, how well it works and how the patient responds. Further tests can be done to find new ways to diagnose or treat a disease.
Complimentary and Alternative therapies: complementary treatments are done to help a person feel better and to alleviate the side effects associated with traditional cancer treatments. On the other hand alternative therapies are offered in place of standard medical care. To avoid any type of dangers or harmful side effects, a cancer patient should consult with a physician prior to trying complementary or alternative treatments for skin cancer.
Basal cell carcinomas rarely spread, but it can invade nearby tissues if left untreated. The choice of treatment will depend on age of patient, tumor size, general health and patient preferences. The following methods have proven successful in basal cell carcinoma treatment; electrodesiccation and curettage, simple excision (cutting out tumor), Mohs surgery (used in treating large tumors when the edges are near the nose, ears, eyes, scalp, forehead, fingers and/or genitals), radiation, immune response modifiers, photodynamic therapy, topical chemotherapy and cryosurgery.
Treating squamous cell carcinomas is done much the same way as basal cell carcinoma treatments, considering the size, tumor location and age and desires of the patient. Larger squamous cell carcinomas are more difficult to treat and the recurrence rate for more aggressive forms can be as high as 50% for deep, large tumors. The following methods can be used to treat squamous cell carcinomas; simple excision, cryosurgery, Mohs surgery, radiation therapy, lymph node dissection and systemic chemotherapy.
Prognosis
The prognosis for skin cancer depends upon many different factors, such as the duration, complications, probable outcome, recovery, survival rates, death rates and other issues. With proper education, early diagnosis and intervention, the factors surrounding the prognosis for skin cancer can change and are unique to each person.
- Photo by steadyhealth.com
- www.medicinenet.com/Melanoma/article.htm
- www.wrongdiagnosis.com/s/skin_cancer/prognosis.htm
- www.medicinenet.com/skin_cancer/article.htm
- cancer.activeskincarepro.com/warning-signs-of-skin-cancer.php
- cancer.activeskincarepro.com/dangers-of-skin-cancer.php
- www.melanomaskincancer.net/9/advice/melanoma-skin-cancer-tests-diagnosis-.html
- www.melanomaskincancer.net/10/advice/nonmelanoma-skin-cancer.html
- www.melanomaskincancer.net/6/advice/melanoma-skin-cancer-causes-and-risk-factors.html