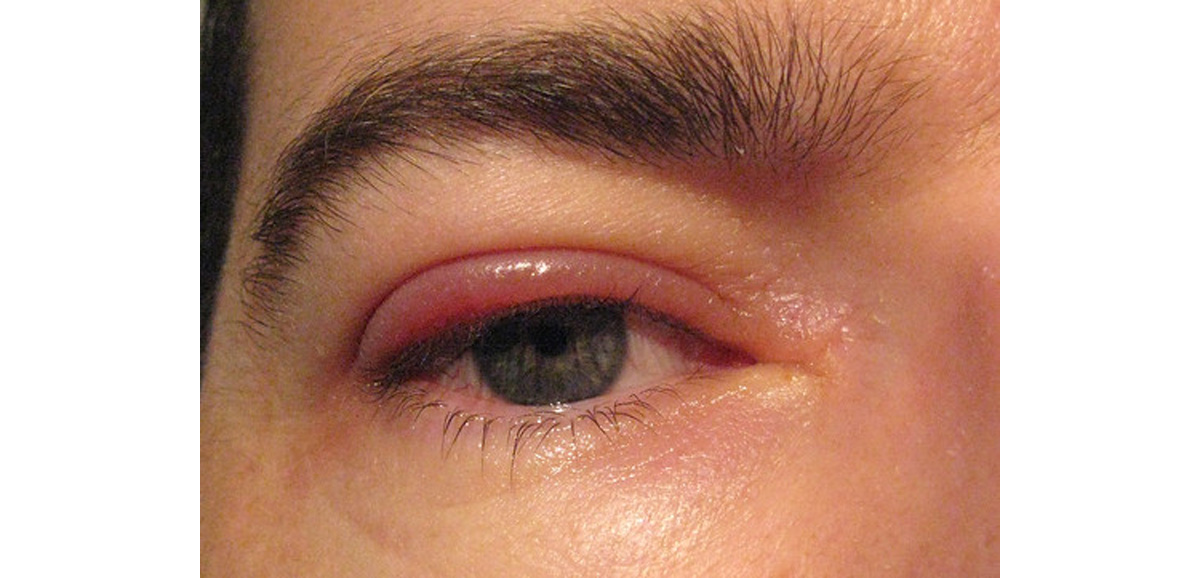
Blepharitis refers to a chronic inflammation of the eyelids. Blepharitis is one of the most common disorders of the eye and is often the underlying reason for eye discomfort, redness and tearing. Other eye symptoms of blepharitis include burning, itching, light sensitivity, and an irritating, sandy, gritty sensation that is worse upon awakening.
There are three main types of blepharitis [1]:
1. Anterior blepharitis:
- the inflammation affects the skin around the base of your eyelashes and it can be caused by either:
- a reaction to Staphylococcus bacteria, which is type of bacterium that usually lives harmlessly on the skin of most people, but for unknown reasons they can cause the eyelids to become inflamed
- seborrhoeic dermatitis – a skin condition that causes the skin to become oily or flakey and sometimes irritate the eyelids, causing the Meibomian glands to block
2. Posterior blepharitis:
- the inflammation affects your Meibomian glands, found along the eyelid margins behind the base of the eyelashes, and it can be caused by either:
- a problem with the Meibomian glands, where the glands get blocked by either debris, skin flakes or inflammation.
- a skin condition called rosacea, which also causes unusual cheek redness.
- seborrhoeic dermatitis.
3. Mixed blepharitis:
- is a combination of both anterior and posterior blepharitis and is the most common type of blepharitis.
There are also several other possible causes that could be connected to blepharitis, such as:
- Herpes simplex dermatitis,
- Varicella-zoster dermatitis,
- Molluscum Contagiosum and
- Allergic or contact dermatitis
Pathophysiology of the condition
The pathophysiology of blepharitis is well understood. It involves simple bacterial colonization of the eyelids. The type of bacteria that is most commonly found in the culture is Staphylococcus aureus. A staph infection of the eyelids results in a direct microbial invasion of tissues, immune system–mediated damage, or damage caused by the production of bacterial toxins, waste products, and enzymes. It is also important to know that colonization of the lid margin is increased in the presence of Seborrheic dermatitis or Meibomian gland dysfunction.
Signs and symptoms of Blepharitis
Generally, there is a persistent and unsightly redness and scaliness of the skin on and around the eyelid margins in patients with blepharitis.
Other signs and symptoms commonly present in cases of blepharitis may include:
- Persistent soreness of the eyelids or eyes.
- The greasy appearance of the eyelid margins.
- Flakes of skin like dandruff.
- Eyelashes that fall out.
- Small ulcers on the eyelid.
- Crusting and bleeding (if severe).
- Irritation of the eye (from flakes).
- The sensation of “something in the eye”.
- Grittiness, burning, itching, and dryness.
- Discharge from the lids, causing lashes to glue together during sleep.
- Sensitivity to light.
- Swelling of the eyelids and conjunctiva.
The eyelids may appear to be greasy and crusted with scales that cling to the lashes. This debris can cause the eyelids to stick together at night, meaning the patient will have trouble opening the eyes on waking up. A patient shouldn’t be concerned if he has to pry his eyes open in the morning because of these sticky secretions. Sometimes, patients may notice only the presence of dried tear secretions in the morning that feel like small grains of sand.
Diagnosis of blepharitis
- Patient’s history
A doctor is usually able to diagnose blepharitis after carefully examining patient’s eyes and eyelids. Sometimes he or she may use a special magnifying instrument during the examination.
- Sample culture
In cases when he or she suspects in bacterial etiology, the doctor may ask for a sample of the skin deposits to be collected to see if any bacteria are present. A bacterial culture, tested in a lab, will confirm the diagnosis if staphylococcal blepharitis.
- Slit lamp examination
This test proved to be very good and effective because it usually shows additional features, including loss of lashes, whitening of the lashes, scarring, and misdirection of lashes, crusting, margin ulcers, telangiectasias, and several other irregularities.
Histological picture of blepharitis
Seborrheic dermatitis has a characteristic histological structure characterized by spongiosis, mild perivascular lymphohistiocytic mononuclear infiltrates in the superficial dermis. It is important to point out that the Staphylococcal blepharitis is a chronic non-granulomatous inflammation, usually with neutrophils.
Complications if left untreated
The most common complications of blepharitis are [2]:
- dry eye syndrome
- loss of eyelashes,
- abnormal eyelash growth or
- scarring of the eyelids
Other possible complications associated with blepharitis include:
- Sty - a bacterial infection that develops near the basic root of an eyelash. It is often accompanied by a painful lump on the edge or inside of the eyelid.
- Chalazion – a condition which occurs when there is some kind of blockage in some of the small oil glands on the eyelid margin
- Excess tearing or dry eyes – it is proven that oily secretions can accumulate in the tear film. This can interfere with the healthy lubrication of eyelids, resulting in very dry eyes or eyes that tear up excessively.
- Chronic pink eye - several studies have proven that blepharitis can lead to recurrent bouts of a pink eye also called conjunctivitis.
- Injury to the cornea - constant irritation may even cause small ulcers which develop on the cornea.
- Meibomian cyst - it develops if one of your Meibomian glands becomes inflamed.
Treatment of blepharitis
Unfortunately, blepharitis is a chronic disease for which there is no cure, and what is most important to know is that it requires long-term treatment to keep it under control. [3]
Treatment consists of 2 phases:
- Acute phase – which involves intensive therapy to rapidly bring the disease under control.
- Maintenance phase - whose goal is to indefinitely continue the minimum amount of therapy that is necessary to keep the disease quiet
- Warm Compresses
Warm compresses have shown very well and effective in the treatment of all kinds of blepharitis and eye infections as well. How do they work? These compresses heat the debris and crust on the lid margin to the melting point of their individual components so that they are easily removed with the lid scrubs. Warm compresses may be combined with eyelid massage. This is especially important in patients who have Meibomian gland dysfunction (MGD). Massaging the eyelid while the compress is on may be very useful.
- Lid Scrubs
Lid scrubbing is a very effective treatment method and there are several ways of performing it. There is only one rule - the scrubbing should only be directed at the base of the eyelashes on the eyelid margin. Soaps used in the process should not have excessive perfume or lotion content. They should be applied with fingertips on the eyelid margin and eyelash bases for up to 1 minute. This is followed by a facial rinse. The soap solution can alternatively be diluted in a container and scrubbing performed using a washcloth wrapped around a finger.
- Antibiotic treatment
The use of an ointment on the eyelid margin immediately after lid scrubbing may help to increase patient’s comfort. Two antibiotics are being used: Erythromycin eye ointment or Tobradex (steroid) eye ointment. These medicines also help to further reduce the bacterial load on the eyelids.
Oral tetracyclines can be used in recalcitrant Meibomian Gland Dysfunction cases for about 3 months.
Oral antibiotics may be prescribed in the presence of a lid abscess or associated rosacea.
- Anti-Inflammatory treatment
Castor oil has been used traditionally for many years as an anti-inflammatory remedy for the treatment of blepharitis. Why is this oil so effective? The main ingredient in it is ricinoleic acid. Patients must know that the eyelid inflammation may increase initially after starting this treatment but with repeated use over the week, the blepharitis inflammation will be reduced.
- Antioxidant treatment
What types of food are rich in antioxidants? The answer is fruits, especially grapes! Eating more grapes may help blepharitis patients. The formation of oxidants like nitric oxide in the involved eyelid margin have been speculated to play a role in blepharitis. A substance known as resveratrol is an anti-oxidant that is very effective against these nitrite types of oxidants. Grapes are particularly good sources of resveratrol. Resveratrol is found in the skin (not flesh) of grapes. Oral N-acetylcysteine treatment for blepharitis needs further evaluation. N-acetylcysteine is a supplement and therefore is available over the counter or in health food stores without prescription.
- Surgical Care
Surgical care for blepharitis is needed only for complications such as:
- chalazion formation,
- trichiasis,
- ectropion,
- entropion, or
- corneal disease.
READ Staph Infection and Pregnancy
- Self-care
It is recommended that patient should deliberately clean eyelid at the base of the eyelashes. To best accomplish this, he or she should gently pull the eyelid away from the eye to avoid accidental injury to the cornea from the washcloth. The treatment should be continued until signs and symptoms disappear. Although you may be able to decrease the frequency of eyelid soaking and washing, every patient should maintain an eyelid care routine to keep the condition under control.
Prognosis
Overall, the prognosis for patients with blepharitis is good to excellent. For most, it remains more of a symptomatic affliction than a true threat to their health and function. It is true that patients experience a considerable amount of discomfort and misery that can greatly reduce their well-being and ability to carry out the daily activities, but recognition of the disease symptoms and appropriate management should help them approach the disease in a successful manner.
- Photo courtesy of jonlarge on Flickr: www.flickr.com/photos/71894657@N00/4338841704/

