But if person who’s planning surgery is among those who have tried and couldn’t lose the excess weight which is causing health problems, weight-loss surgery may be an option. The principal role of any gastrointestinal surgery for obesity, also called bariatric surgery, is to alter the digestive process.

Restrictive: These operations limit food intake by creating a narrow passage from the upper part of the stomach into the larger lower part, reducing the amount of food the stomach can hold and slowing the passage of food through the stomach.
Mal-absorptive: These operations do not limit food intake, but instead exclude most of the small intestine from the digestive tract so fewer calories and nutrients are absorbed. Mal-absorptive operations, also called intestinal bypasses, are no longer recommended because they result in severe nutritional deficiencies.
Combined restrictive/mal-absorptive: Combined operations use stomach restriction and a partial bypass of the small intestine.
It is, however, important to point out that surgery is not a definite solution to the problem of morbid obesity, but rather an emergency action in order to prevent the development of secondary conditions and complications. Patients should not be lead to believe that all problems will be gone once they have undergone surgery.
Restrictive types of weight loss surgery
Purely restrictive operations for obesity include adjustable gastric banding (AGB) and vertical banded gastroplasty (VBG).
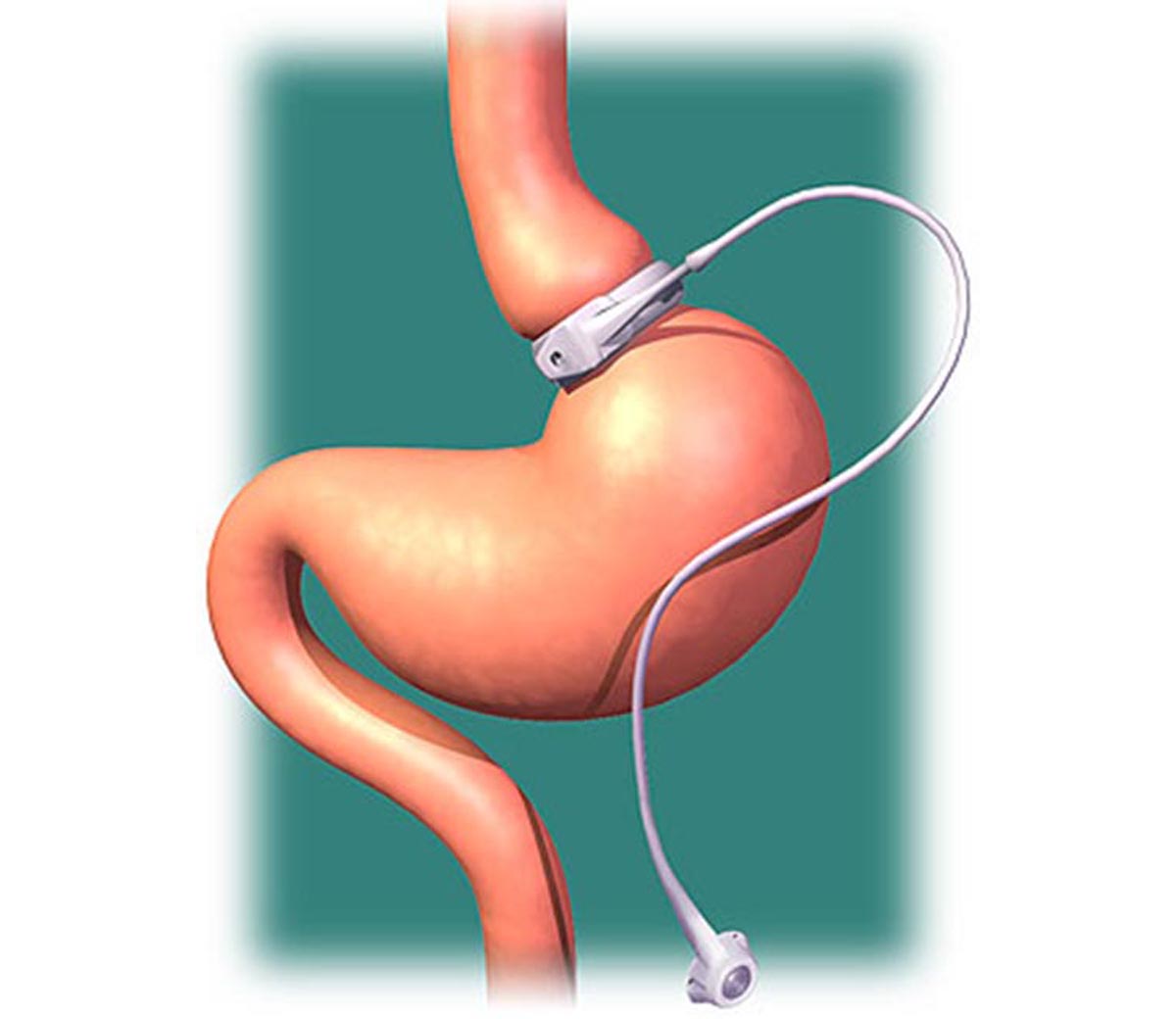
- Adjustable gastric banding: A hollow band made of silicone rubber is placed around the stomach near its upper end, creating a small pouch and a narrow passage into the rest of the stomach. The band is then connected with a salt solution through a tube that connects to an access port placed under the skin. It can be tightened or loosened over time to change the size of the passage by increasing or decreasing the amount of salt solution.
- Vertical banded gastroplasty: This operation uses a band and staples to create a small stomach pouch. This was once the most common restrictive operation, but today it is no longer frequently done.
Combined weight loss operations
Combined operations are the most common bariatric procedures. They are also the most effective because they restrict both food intake and the amount of calories the body absorbs.
Roux-en-Y gastric bypass (RGB): This operation is the most common and successful combined procedure in the United States. The surgeon creates a small stomach pouch to restrict food intake after which a Y-shaped section of the small intestine is attached to the pouch to allow food to bypass the lower stomach, the duodenum, and part of jejunum, reducing significantly the amount of calories and nutrients the body absorbs.
Biliopancreatic diversion (BPD): This is a far more complicated operation in which the whole lower portion of the stomach is removed. The small pouch that remains is connected directly to the final segment of the small intestine, completely bypassing the duodenum and the jejunum. Although this procedure leads to weight loss, it is used less often than the other types because of the high risk for nutritional deficiencies
Laparoscopic Bariatric Surgery
Gastric bypass operation
Gastric bypass surgery literally changes the anatomy of the digestive system in order to limit the amount of food a person can eat and digest. Most surgeons prefer this procedure because it's safer and has fewer complications than other available weight-loss surgeries. This is a major procedure that poses significant risks and side effects.
Indications
Gastric bypass surgery is reserved for people who are unable to achieve or maintain a healthy weight through diet and exercise. It is also indicated for the severely overweight, and those who have health problems as a result.
Gastric bypass may be considered if:
- body mass index (BMI) is 40 or higher (extreme obesity)
- BMI is 35 to 39 (obesity)
- There are several weight-related health problems such as diabetes or high blood pressure
It is extremely important to understand that no weigh loss surgery replaces the need for following a healthy diet and regular physical activity program.
Preparations for the operation
A patient should be psychologically and medically ready for the surgical procedure. This involves identifying which aspects of health can be expected to improve after surgery, and what aspects of health may increase the risks of surgery. The surgery may not be recommended or may be postponed if there's any sign that a patient is not psychologically or medically ready for the procedure. Just before the operation, there are several restrictions such as limited eating, drinking, starting a program of physical activity, and limiting or stopping the use nicotine products.
READ Clinical Trial Confirms: Experimental Weight Loss Drug Lorcaserin Works
The procedure
The surgeon staples the patient’s stomach across the top, sealing it off from the rest. As a result, the gastric pouch is about the size of a walnut and can hold just about an ounce of food. This bypass redirects food, skipping most of the stomach and the first section of the small intestine (duodenum). Food enters directly into the second section of small intestine (jejunum), limiting your ability to absorb calories.
Every gastric bypass surgery is performed under a general anesthesia, and the whole operation takes about four hours. Sometimes hospital stay may last from three to five days. Following the month of liquid diet, the patient is advised to eat mashed food, and thereafter use small portions of normal food.
Post-operative expectations
The patient will not be allowed to eat for one to two days after the surgery so that the stomach can heal properly. After this period the patient will follow a specific dietary progression for about 12 weeks. This begins with liquids only, proceeds to pureed and soft food, and finally to regular food. In the first six months after surgery, eating too much or too fast may cause vomiting or an intense pain under the breastbone.
Some patients may experience one or more of the following changes in the first three to six months:
- Tiredness
- Chills
- Dry skin
- Hair thinning and hair loss
- Body aches
- Mood changes
Within the first two years of surgery, a patient can expect to lose 50 to 60 percent of excess weight. The period after surgery until the weight is stabilized has to be regarded as a period of relative starvation. It is not advisable to become pregnant during starvation, because the child may suffer from this. When weight loss is completed, there is no contraindication to pregnancy. All tablets that the patient is using should be divided into small pieces or crushed before they are taken with water. It is very common that changes in medication for hypertension, diabetes, asthma or other diseases may be necessary during the period of rapid weight reduction.
Vomiting
Vomiting is also a very common complication of all gastric bypass operations. Most patients will feel pain or the vomit impulse after intake of food. This is in most cases caused by eating too much and too quickly. If eating is slow and calm, patients will learn to listen to the signals from the stomach. Regular vomiting is a sign of warning. This can either be caused by wrong eating behavior or the outflow of the gastric pouch becoming too narrow.
How much do these operations cost?
Bariatric procedures cost from $20,000 to $35,000. Medical insurance coverage varies by state and insurance provider. If the patient is considering bariatric surgery, he or she should contact a regional Medicare or Medicaid office or insurance plan to find out if the procedure is covered.
- www.win.niddk.nih.gov
- en.wikipedia.org/wiki/Bariatric_surgery
- http://www.webmd.com/diet/weight-loss-surgery/weight-loss-surgery-frequently-asked-questions
- www.surgicalteam.com
- image: www.akrongeneral.org
- www.piyavate.com

