Table of Contents
Are you very obese and have more traditional attempts at weight loss not offered you the results you were looking for? You are not alone — once you are 100 lbs or so above a healthy weight, diet and exercise alone will often not be enough. An increased stomach size means you will constantly be feeling hungry, and exercise will soon result in shortness of breath and severe physical pain.
Bariatric surgery may make all the difference, giving you a fresh start to your weight loss journey. It's not for the faint-hearted and certainly no easy way out, though. If you have been toying with the idea of talking to your doctor about weight loss surgery, here is some food for thought.
What Is Bariatric Surgery?
Bariatric surgery, on the most basic level, is surgery designed to promote weight loss in morbidly obese people. This can be done by reducing the size of the stomach or by altering the small intestine in such a way as to interfere with the normal absorption of calories and nutrients. Both types of bariatric surgery change a person's physical interaction with food on a very basic level.
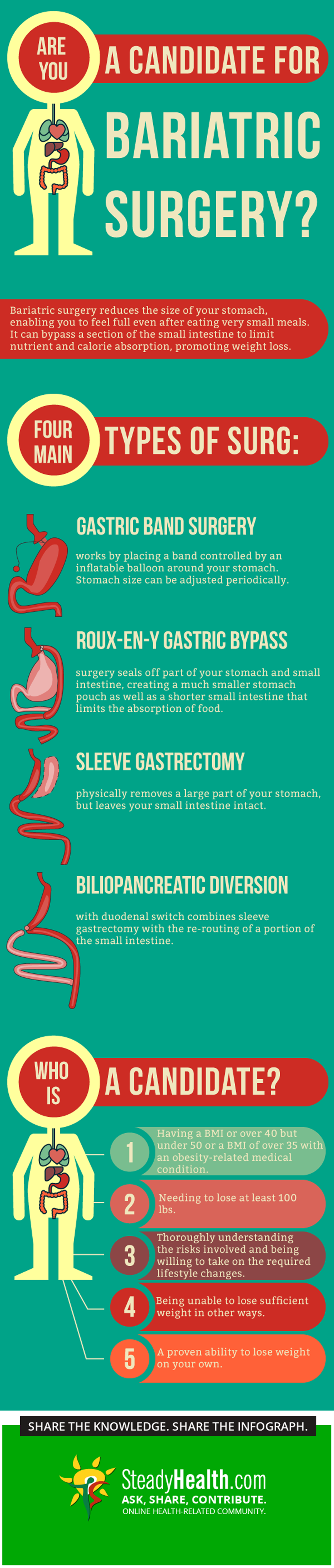
Gastric band surgery, for instance, limits the amount of food the stomach can hold by putting a band controlled by an inflatable balloon in place around the stomach. Connected to a port right under the abdominal skin, this set-up can then be adjusted at a later date. This surgery neither alters digestive function by bypassing a portion of the small intestine, nor reduces the size of the stomach — it just makes the active, used part of the stomach smaller.
Roux-en-Y gastric bypass is a more radical surgery. Though this surgery doesn't physically remove any part of the digestive tract, it alters the usable portions of the stomach and small intestine. This surgery sections off a small portion of the stomach to create a "pouch", to which the small intestine is then attached. Because part of the small intestine remains with the original larger stomach, post-surgery patients can't absorb as many nutrients. With their new smaller stomach, they can also eat much less.
In a sleeve gastrectomy, the size of the stomach is reduced by completely removing part of it. The operation gets is name from the fact that the new stomach looks somewhat like a small sleeve. Though a sleeve gastrectomy doesn't impact the small intestine in any way, the much smaller stomach patients are left with also emits less of the hunger hormone grehlin, helping the patient control their eating patterns by reducing their appetite.
A biliopancreatic diversion with duodenal switch combines sleeve gastrectomy surgery with re-routing a portion of the small intestine to limit nutrient absorption. Because the relevant portion of the small intestine is re-routed rather than removed, however, bile and pancreatic digestive juices can still flow freely.
All types of bariatric surgery end with a smaller functional stomach, which means that you can eat much less and still feel satisfied. Bariatric surgery that also alters the digestive process results in faster weight loss, but this also means that you are at a greater risk of nutritional deficiencies. More about that later.
Risks Of Bariatric Surgery
Like all types of surgery, bariatric surgery carries risks. Some, such as pulmonary embolism, deep vein thrombosis, and internal hemorrhage can be fatal. Bariatric surgery is especially risky for people in the super-morbidly obese category, and few surgeons will work with people with BMIs exceeding 50 for this very reason. However, because remaining in that weight category carries very high risks in itself, some bariatric surgeons believe that the benefits of surgery outweigh the risks, and will perform weight loss surgery even on super-morbidly obese people.
Before you undergo weight loss surgery, it is very important to understand both the short-term risks of the surgery and the impact it will have on the rest of your life.
- Infographic by SteadyHealth.com


Your thoughts on this