There are four main types of thyroid cancer:
- Papillary thyroid cancer: This is the most common form of thyroid cancer arising from the follicular cells. Almost 86 out of every 100 cases diagnosed as thyroid cancers are of this type. Papillary thyroid cancer is a slow growing tumor and generally responds well to treatment.
- Follicular thyroid cancer: It is the second most common type of thyroid cancer and represents 9 out of every 100 cases of thyroid cancer. This tumor also shows good response to treatment.
- Medullary thyroid cancer: 2 out of every 100 cases of thyroid cancer are of medullary type. They arise from the C cells and produce large quantities of calcitonin. They are slow going tumors and can be treated if caught early.
- Anaplastic thyroid cancer: This type of thyroid cancer is extremely rare affecting 1 in every 100 cases of thyroid cancer. The tumor arises from the follicular cells, is fast growing in nature and metastasizes early. Therefore, these type of tumors are the most difficult to treat.
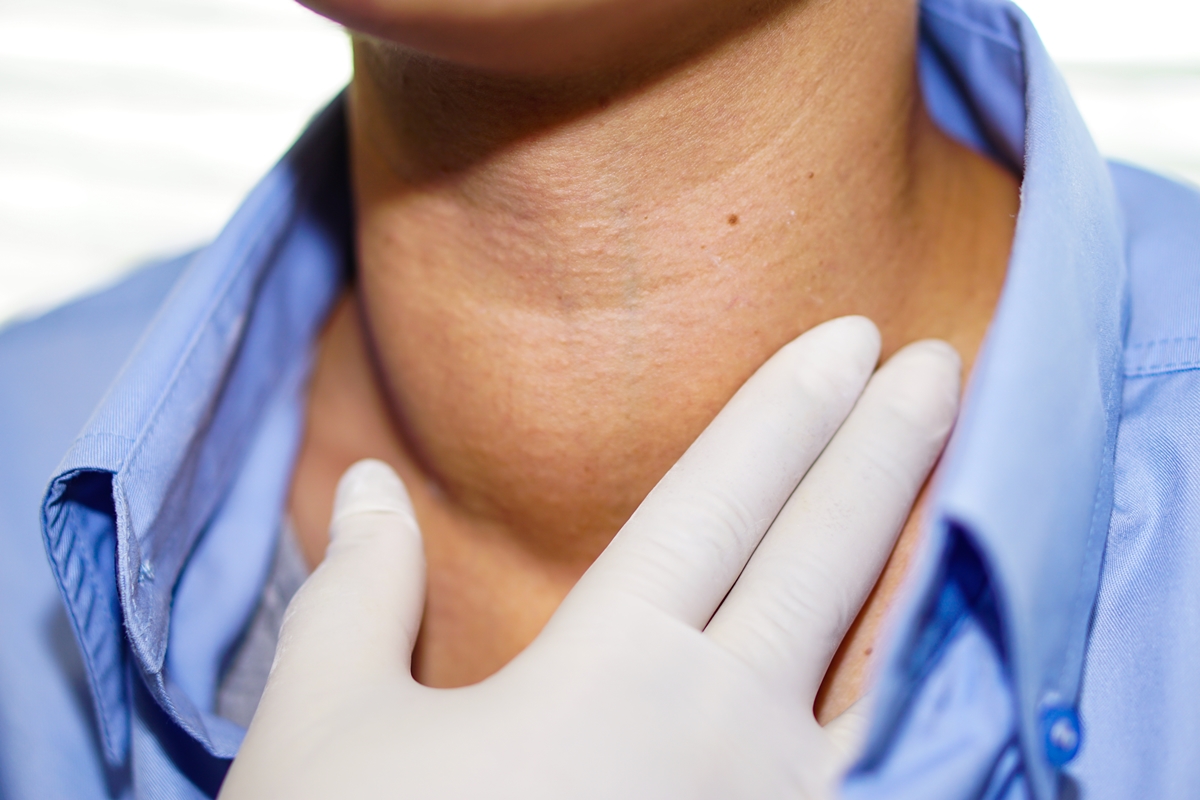
The treatment of thyroid cancer usually involves:
- Surgery
- Chemotherapy
- Hormonal therapy
- External beam radiation therapy
- Radioactive iodine therapy
- Targeted therapy
The goal of the therapy is to remove the tumor completely along with the lymph node which may be possibly infected. Usually two or more treatment modalities mentioned above are employed to achieve the best possible results. However, despite the best treatment, there are chances of recurrence of the tumor, even 10 to 20 years after the initial treatment. This is especially true when the tumor is detected at an advanced stage or is of a more malignant nature, like the anaplastic thyroid tumor. Therefore, the patients who have undergone treatment for thyroid cancer are asked to come for follow-up visits where they are subjected to ultrasounds and radio-iodine scans to look for any evidence of recurrence.
Follow up in case of papillary or follicular thyroid cancer: The patients, whose thyroid gland has been removed as a part of treatment of papillary or follicular cancer, are made to undergo a radioactive iodine scan 6 to 12 months after the initial treatment. If the results come as negative, no further scan is required unless there are any other symptoms. Their thyroglobulin and TSH levels are also tested. If the thyroglobulin levels show an increase, it could signify a recurrence and the patient is subjected to PET scans and other imaging tests.
Follow up in case of medullary thyroid cancer: The levels of calcitonin and carcino-embryonic antigen (CEA) are tested. It they show a rise, ultrasound of neck, CT scan and a MRI scan are done to find any evidence of recurrence.
Further treatment in case of recurrence depends upon the following factors:
- Cell type
- Uptake of radioactive iodine
- Treatment undertaken earlier
- Site of recurrence
- Condition of the patient
There are three types of recurrence:
- Local recurrence
- Regional recurrence
- Distant recurrence
Local recurrence: In case of local recurrence, surgery for removing remaining lymph nodes, followed by radio-active iodine treatment, is effective in controlling the disease in more than 70% cases.
Regional recurrence: Modified radical neck dissection is the best approach to deal with regional recurrence.
Distant recurrence: Distant metastasis usually occurs to lungs, bones or brain. Local therapies like radiation and ethanol injections may be considered. Chemotherapy is used in advanced cases.









-In-Infants-And-Older-Children_f_280x120.jpg)