Table of Contents
Cellulite is an interesting medical condition: it gives lots of troubles and worries to millions of women around the world, but it never jeopardizes anyone’s health. In fact, most physicians do not recognize cellulite as a disease, instead referring to it as to an unaesthetic skin architecture alteration in women after puberty. However, a short overview of scientific literature provides a slightly different perspective to the problem and links it to the problem of obesity.
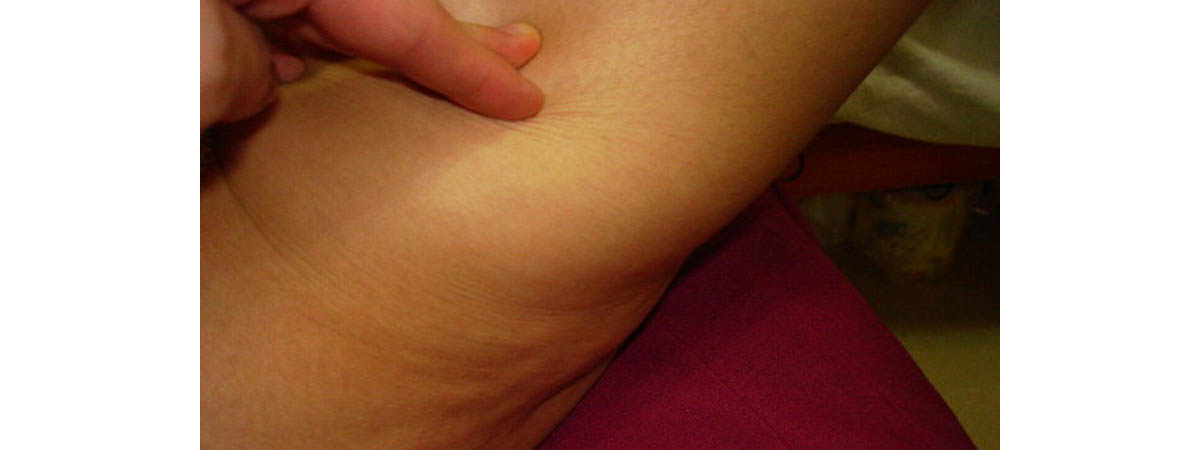
What is cellulite?
Although the condition is known from prehistory, the first scientific description of cellulite was done only in 1920. It explained cellulite as a complex dystrophy of subcutaneous tissue caused by incorrect water metabolism. Later publications defined cellulite a localized metabolic disorder of subcutaneous tissue or even a complex psychosomatic disorder.
Cellulite is common: it is observed in 90-98% of all non-Asian post-pubertal women and runs in families suggesting strong genetic component. Genetic studies show that mutation in angiotensin-converting enzyme which is involved in blood pressure regulation and tissue swelling development acts as a major genetic risk factor for cellulite.
It is intriguing that despite the significant concerns caused by cellulite, there was very little research on this condition since it was described by French doctors Alquier and Paviot. Tons of popular publications about cellulite were produced but only a very limited number of peer-reviewed articles presenting the data on cellulite causes, risk factors and pathophysiology was published over the years.
Here I’m attempting to analyze the available peer-reviewed scientific publication to get some insight to cellulite and its treatments.
Scientific view on what’s under the skin
Subcutaneous tissue that gets altered during the cellulite development is the third deepest layer of skin. This tissue is composed of cells such as fibroblasts and myofibroblasts that produce the connective fibre molecules. In addition, the tissue is populated with mature and immature fat cells and also contains immune cells, blood vessels and nerves. Just a third of all cells in subcutaneous tissue are the mature fat cells.
Scientists use a different, more specific name for cellulite – ginoid lipodystrophy. This name points to the direct involvement of female hormone (estrogen) as a major player in the cellulite development. Pathological symptoms of cellulite include the swelling of subcutaneous tissue (edema), chronic venous insufficiency (defective micro-circulation of lymph in affected areas), abnormal hyper-polymerization of the connective anchoring fibers, decreased skin surface temperature in affected areas, and changes in fat cells metabolism.
Pathologists do understand now how cellulite develops. It starts with the blood circulation problems that lead to alteration of lymph passing through capillary wall. As a result, water retains in tissue causing swelling. On the following step, the persistent swelling leads to changes in the subcutaneous connective cells metabolism. These cells become enlarged and abnormally increase in number. These larger and more numerous cells start to invade available space between subcutaneous fat cells. They also start overproducing the scaffold–forming fiber molecules. Fiber molecules such as collagen naturally tend to bind to each other. During the cellulite development, the overproduced fibers bind together and form the irregular structures that encapsulate the groups of fat cells thus forming nodules of different sizes. Eventually, these small nodules fuse together giving rise to bigger structures and start thickening and hardening (the process known as sclerosis).
All blood vessels are surrounded by specialized fat cells called perivascular cells. These cells produce important regulatory chemical compounds such as growth factors for fibroblasts and factors regulating vascular tone. Excessive fat cells number due to the weight gain may cause arterial stiffness, blood vessel wall rigidity and decreased vein dilation leading to local decrease in blood supply. It was recently shown that in females the fat cells are producing a number of hormones including sex hormone estrogen. Estrogen production by fat cells increases with the increase of body weight. Estrogen amount rises up at the site of synthesis and promotes growth of surrounding fatty tissue due to its steroid responsiveness. This initiates a vicious circle: estrogen causes more weight gain, which in turn causes more estrogen production, faster fat cell growth, and even more estrogen produced, and so on. Also, the larger amounts of other regulatory chemicals get produced as well. Then further steps get initiated. Blood vessels get stiffer and not dilated, lymph stagnates in surrounding tissue, and the swelling evolves. The connective tissue cells multiply and get bigger in size, invading empty spaces and producing more building material for fibers. Fibers bind together and form irregular structures typical for cellulite. Scientific studies clearly indicate that cellulite is clinically more evident with weight gain.
Subcutaneous tissue has septa formed by connective fibers. Most of those septa are parallel or oriented under 450 angles to skin surface in healthy people. When the cellulite-associated changes in blood supply, hormonal status, swelling, and connective cell overgrowth occur, the newly formed septa positions are also altered. Perpendicular septa pattern develops. Some reports state that thickness of septa is decreased. It means that lesser and thinner septa parallel to the skin surface cannot efficiently smooth the fat protruding through the upper skin layers but perpendicular patterns help the extra fat cells to rise up as a dough in cupcake forming the typical and noticeable fat bulges.
Risk factors for development of cellulite include the unbalanced or poor diet (diet rich in fat and carbohydrates, poor in fibers and proteins), inactive lifestyle, decrease in muscle mass, as well as some inherited genetic features.
- Emanuele E. (2011) Toward a molecular understanding of cellulite: facts, controversies, and future directions. J Am Acad Dermatol. 64(2):439
- Wassef C, Rao BK (2012) The science of cellulite treatment and its long-term effectiveness. J Cosmet Laser Ther. 14(2):50-8
- Khan MH, Victor F, Rao B, Sadick NS (2010) Treatment of cellulite: Part I. Pathophysiology. J Am Acad Dermatol. 62(3):361-70
- Khan MH, Victor F, Rao B, Sadick NS (2010)Treatment of cellulite: Part II. Advances and controversies. J Am Acad Dermatol. 62(3):373-84
- Pugliese PT (2007)The pathogenesis of cellulite: a new concept. J Cosmet Dermatol. 6(2): 140-2
- Rosenbaum M, Prieto V, Hellmer J, Boschmann M, Krueger J, Leibel RL, Ship AG (1998)An exploratory investigation of the morphology and biochemistry of cellulite. Plast Reconstr Surg. 101(7): 1934-9
- Rossi AB, Vergnanini AL. (2000)Cellulite: a review. J Eur Acad Dermatol Venereol. 14(4): 251-62.
- Photo courtesy of MikeMunoz39 by Wikimedia Commons : commons.wikimedia.org/wiki/File:Leg_cellulite.jpg
- Photo courtesy of dion gillard by Flickr : www.flickr.com/photos/diongillard/2460491143/


Your thoughts on this