Table of Contents
Rheumatoid arthritis is a systemic, chronic disease in which the synovial joints of the body, most commonly in the fingers, and the knees and hips, become inflamed. Over time, erosion of the bone occurs and nodules form under the skin, resulting in painful swelling and joint deformity. Rheumatoid arthritis has no cure. Treatment is focused on alleviating symptoms and heading off damage to the joints.
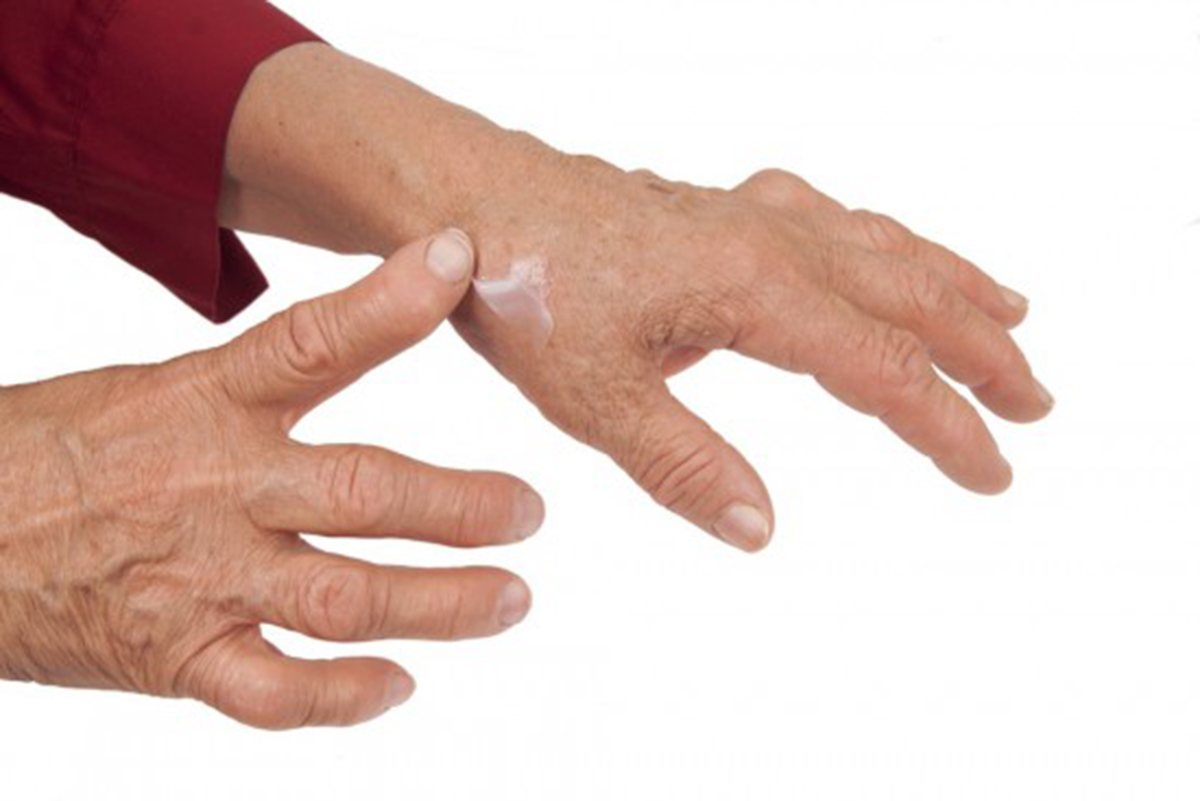
What Causes Rheumatoid Arthritis?
The exact cause of rheumatoid arthritis is unknown, but it is an autoimmune disorder.
When something happens to this tolerance, your body can stop recognizing its own cells and will begin to attack them, resulting in inflammation and destruction of the tissue it no longer recognizes.
Although, there isn't a clear genetic link for rheumatoid arthritis, your genes do seem to have some role in your chances of developing the disease. Native Americans, among other ethnic groups, have a higher rate of rheumatoid arthritis than the general population. Women of all ethnic groups are three times more likely to have the condition than men. And while rheumatoid arthritis can develop at any age, most people experience their first symptoms between the ages of 40 and 60.
The Symptoms
The most obvious symptom is joint pain, especially in the morning or after periods of rest.
Rheumatoid arthritis is a systemic disease, though, so symptoms can develop throughout the body. Those living with the disease may also have fluid buildup in the lungs and within the heart. The disease can progress gradually over several months or symptoms can arise abruptly.
How to Treat Rheumatoid Arthritis
As a chronic condition, there is no cure for rheumatoid arthritis. Treatment is focused on managing the pain and trying to prevent or slow down the destruction of the joints.
The first line of defense is usually over-the-counter medication. NSAIDs (nonsteroidal anti-inflammatory drugs) such as ibuprofen (Motrin or Advil) and naproxen sodium (Aleve) help to relieve both pain and inflammation. Long-term use can lead to serious side effects such as inflammation of the upper gastrointestinal tract and bleeding, especially in the elderly.
During flare-ups, your doctor may prescribe a corticosteroid to relieve the worst of the symptoms before gradually tapering the medication off to avoid the serious possible side effects of osteoporosis, diabetes, and cataracts.
Read More: Rheumatoid Arthritis Makes It Difficult to Conceive
Medications in the disease-modifying antirheumatic drugs class (DMARDs) include hydroxychloroquine (Plaquenil) and methotrexate (Trexall) and must be taken for several months before their full effects are apparent.
Medications such as etanercept, infliximab, and adalimumab are particularly effective when combined with traditional DMARDs. They are administered through injections or infusions and require close monitoring for infections and other serious side effects.
Powerful immunosuppressive drugs such as Cyclosporine and mycophenolate may be used in conjunction with DMARDs or other drugs to battle the systemic effects of rheumatoid arthritis, but these drugs can increase your risk of infection since they work by suppressing your immune system.
Most radically, joint replacement surgery may be most helpful for some patients. Surgical options for chronic arthritis include joint repair to realign or mend joints, often using minimally invasive techniques for quicker recovery. Joint replacement, especially for hips and knees, replaces damaged joints with artificial ones, significantly reducing pain and improving mobility. Joint fusion, used in smaller joints, fuses bones to form a rigid unit.
- Rheumatoid arthritis. (2001). In Taber's Cyclopedic Medical Dictionary (pp.166-167, Edition 19). Philadelphia, PA: F. A. Davis Company.
- Photo by shutterstock.com
- Photo courtesy of Domas Mituzas by Flickr : www.flickr.com/photos/midom/328087524/
- www.universaldesign.com
- www.arthritis.org


Your thoughts on this