Rheumatoid arthritis (RA) is a chronic inflammatory autoimmune disorder that is caused by the immune system producing antibody proteins that attack the synovium that lines the joints. This disease can also affect a wide variety of systems such as the eyes, skin, lungs, heart and blood vessels.
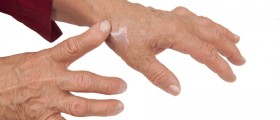
Unlike osteoarthritis that occurs due to wear-and-tear that mainly affects the weight bearing joints, RA affects the lining of the joints which causes a painful swelling that may result in erosion of the bone and subsequent deformity of the surrounding bony anatomy.
Causes
The antibodies that attack the synovium cause inflammation that results in this tissue becoming thicker, and this can lead to destruction of the cartilage and bone surrounding the affected joints. The ligaments and tendons that offer support to the joint weaken and stretch, and this results in deformity of the joint.
The exact cause of RA is not clearly understood, but the theory is that a genetic component is linked to the development of this debilitating condition.
Risk factors
The following factors may increase the risk of developing RA.
- Females are more likely than males to develop RA.
- Being between the ages of 40 and 60.
- Having a family history of the condition.
- Smoking cigarettes.
- Exposure to products such as silica or asbestos.
- Obesity, especially in females diagnosed with RA before 55 years of age.
Symptoms
Symptoms and signs of RA may include:
- Swollen, warm or tender joints.
- Stiffness of the joints that's worse in the mornings or after being inactive.
- Weight loss, fever and fatigue together with the above issues.
Complications
RA or the medications used to treat the condition can cause the following complications.
- Osteoporosis, with an increased risk of sustaining fractures.
- Infections, due to an impaired immune system.
- Rheumatoid nodules.
- Abnormal body composition.
- Dry mouth and eyes, due to Sjogren's syndrome.
- Lung disease, such as emphysema.
- Heart problems, such as pericarditis.
- Carpal tunnel syndrome.
Diagnosis
RA can be difficult to diagnose because the symptoms it causes are non-specific to this disease. There are no specific blood tests that can diagnose it either, but rather suggest its presence when correlated with significant clinical findings.
Blood tests
- Increased C-reactive protein (CRP).
- Increased erythrocyte sedimentation rate (ESR).
- Positive rheumatoid factor (RF).
- Positive anti-cyclic citrullinated peptide (anti-CCP) antibodies.
Imaging tests
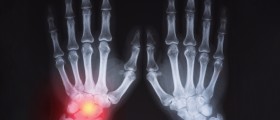
- X-rays can show bony erosions.
- MRI and ultrasound can be done to assess the severity of the disease.
Management
There is no cure for RA, but medications such as the disease-modifying anti-rheumatic drugs (DMARDs) are known to result in remission of the condition.
Medications.
- Non-steroidal anti-inflammatory drugs (NSAIDs).
- Corticosteroid medications.
- Disease-modifying anti-rheumatic drugs (DMARDs), which slow the progression of RA and protect the joints and other tissues from permanent damage.
- Biologic agents, which target parts of the immune system that cause inflammation which results in tissue and joint damage.
Therapy
- Physical or occupational therapy to teach you exercises to help keep the joints flexible.
Surgery
If the medications can't slow down disease progression, then surgical intervention may be needed to replace damaged joints.
RA surgery may involve one or more of the following procedures:
- Synovectomy - removing the inflamed synovium.
- Tendon repair.
- Joint fusion.
- Total joint replacement.
Alternative medicine
Alternative treatments that have shown some benefit for patients with RA include:
- Fish oil (omega-3).
- Plant oils.
- Tai chi - a movement therapy involving gentle stretches and exercises combined with deep breathing.