Table of Contents
Type 1 Diabetes and Celiac Disease are both autoimmune conditions, disorders where your body's immune system attacks itself. In Celiac Disease, your autoimmune system attacks the lining of your small intestine, preventing your body digesting nutrients. In Type 1 Diabetes, your body attacks the pancreatic cells, preventing your body's natural production of insulin.
What is Type 1 Diabetes?
Type 1 Diabetes is the genetic form of Diabetes (as opposed to Type 2 Diabetes, which is often caused or exacerbated by lifestyle). It is usually diagnosed in children, although environmental factors can lead to destruction of Beta Cells in the pancreas, and lead to the development of Type 1 Diabetes in later life. Of 415 million diabetics worldwide, approximately 10% have Type 1 Diabetes.
Symptoms include: fatigue, thirst, frequent urination, hunger, weight loss, and dry mouth.
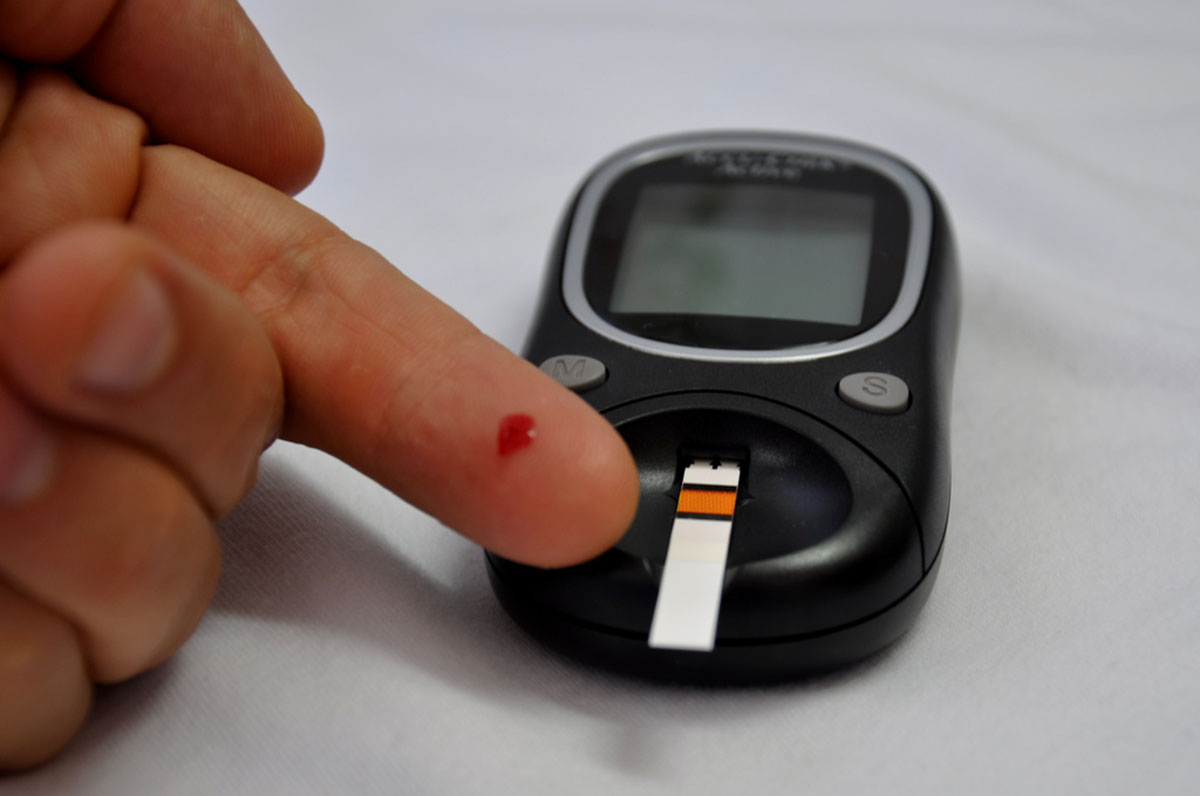
Diabetes is easier to test for than Celiac Disease. All it requires is a fasting blood test that measures how much glucose is in the blood. A certain level of glucose shows that an individual is diabetic or pre-diabetic. Another, highly reliable blood test is called the Glycated Haemoglobin (HbA1c) test. This measures your long-term blood glucose control, and may be a more accurate way at measuring your average glucose levels over a long period of time.
Treating Type 1 Diabetes involves following a healthy diet, and taking regular insulin injections.
What is Celiac Disease?
Celiac Disease is another inheritable condition, where eating gluten triggers the body's immune system to react as though it was being attacked by a foreign body. In Celiac Disease, the body perceives gluten as a threat, and responds accordingly. An estimated 1 in 100 people have Celiac Disease, according to current research.
Symptoms of Celiac Disease include: foul-smelling diarrhoea, bloating, flatulence (breaking wind), abdominal pain, fatigue, children not growing as they should.
Diagnosis is made by two methods: an initial blood test to screen potential sufferers, and a biopsy of the small intestine to confirm diagnosis. The blood tests for celiac antibodies. If antibodies are found, you will be sent for a colonoscopy and biopsies will be taken, which will confirm the diagnosis.
The only treatment for Celiac Disease is a strict, lifelong gluten-free diet.
So is there a link?
While no link has been established between Type 2 Diabetes and Celiac Disease, a link between Type 1 Diabetes and Celiac Disease has been suspected since 1960.
A study of children with Diabetes Type 1 (Barera et al, 2001) tested 273 children for Celiac Disease and found Celiac Disease present in 3.3% of their test population, more than the 1% of the general population. It has even been theorised by Hansen et al that, by the mother following a gluten-free diet throughout pregnancy and breastfeeding, she minimises the chance of her offspring developing Type 1 Diabetes.
READ Type 1 Diabetes and Getting Ready for Pregnancy
A further study demonstrated an 8% prevalence of Celiac Disease in patients with Type 1 Diabetes. They discovered that the Celiac Disease was more likely to be asymptomatic in patients with Type 1 Diabetes, or that patients may have symptoms that are confused with diabetes.
Other research has reported that between 4.4% and 11.1% of patients with Type 1 Diabetes also have Celiac Disease. The reverse is also true. Type 1 Diabetes has been found in 2-10% of all celiacs, more than the usual 0.75% of the population.
- http://care.diabetesjournals.org/content/26/6/1932.full https://celiac.org/celiac-disease/cd-and-diabetes http://www.celiac.com/articles/23010/1/Celiac-Disease-in-Type-1-Diabetes-Mellitus/Page1.html http://www.celiac.com/articles/23701/1/Can-a-Gluten-free-Diet-Lower-the-Risk-of-Diabetes/Page1.html http://www.celiac.nih.gov/CDandDiabetes.aspx https://www.coeliac.org.uk/coeliac-disease/associated-conditions-and-complications/type-1-diabetes https://www.coeliac.org.uk/coeliac-disease/myths-about-coeliac-disease http://www.diabetes.co.uk/diabetes-and-coeliac.html https://www.diabetes.org.uk/Guide-to-diabetes/Monitoring/Testing/#HbA1c https://www.diabetes.org.uk/Documents/Position%20statements/Diabetes%20UK%20Facts%20and%20Stats_Dec%202015.pdf http://www.nhs.uk/conditions/Coeliac-disease/Pages/Introduction.aspx http://www.nhs.uk/Conditions/Coeliac-disease/Pages/Diagnosis.aspx http://www.sciencedaily.com/releases/2008/12/081210180841.htm http://www.webmd.com/digestive-disorders/celiac-disease/news/20081210/celiac-disease-type-1-diabetes-linked
- Photo courtesy of v1ctor: www.flickr.com/photos/v1ctor/10871254373/
- Photo courtesy of Nicola since 1972: www.flickr.com/photos/15216811@N06/7304112900/


Your thoughts on this