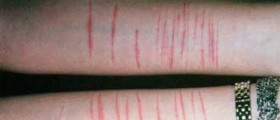
Cutting oneself without wanting to and despite the desire to stop and making efforts to stop is part of a disorder of harming oneself that has been recognized since ancient times and in most cultures and societies. Western medicine and psychiatry classed self-harm with suicide attempts for a long time, but it is now recognized that cutting and other forms of self-injury are not a form of suicide or suicide attempt, although over time the injuries can have bad or even fatal outcomes. In its 2013 revision of the Diagnostic and Statistical Manual of Mental Disorders that is used to identify and classify psychiatric conditions, the American Psychiatric Association identified repeated cutting or other self-injury as a separate disorder, Non-suicidal Self Injury. There are a number of approaches to dealing with this problem; anyone with this condition who wants to get better will have to take some kind of step toward treatment, but treatment need not be complicated or expensive or public.

Non-suicidal self-injury is characterized by five or more days in a year with self-inflicted injury, without the desire to commit suicide but with the wish to escape from a negative feeling state, achieve a positive feeling state or resolve some interpersonal problem. Eighty per cent of people who harm themselves do so by cutting or stabbing the skin. The intent or desire to commit suicide is very rare; for that matter, the old term of "self-mutilation" is also inaccurate because almost no one with the condition really wants to disfigure herself or himself. It was thought for a long time that people did this in order to get attention, but studies show that most people are self-conscious about their wounds and scars, may feel guilty about this self-injury and often try to conceal this from others. Cutting is most often a symptom of depression, bipolar disorder or disorders of conduct or personality and is also seen with some neurological conditions. Childhood abuse, difficult relations with a parent or a partner, intense grief and bereavement and being involved in a very bad social or economic situation are among the main precipitating factors. Alcohol and drug use and withdrawal, particularly benzodiazepines such as Valium or Xanax, can bring on self-injury or make it worse; using cannabis, even though it is associated with other health and emotional problems, does not seem to be a factor for self-harm.
It has been suggested that endorphins in the brain, natural pain-relieving, pleasure-enhancing and tension-relieving chemicals that are released by the brain in response to injury or pain medications, may be decreased in amount or deficient in effect in people who self-injure, and that stimulation of the sympathetic nervous system and increased release of endorphins may be the effect of injury. Physical pain may therefore help to alleviate the feelings caused by psychological pain. People who self-harm often report the inability to experience pleasure (anhedonia) or feelings of emptiness and numbness; it has been suggested that the unpleasant feelings after self-injury are actually a way of feeling something, and may be better than no feelings at all.
Many people who cut or otherwise self-injure are reluctant to seek treatment, but it is a serious problem and the World Health Organization estimates that 800,000 people a year die from the effects of untreated self-injuring. The simplest approach to treatment may not involve public diagnosis and therapy at all; substituting alternative behaviors for cutting has been shown to be an effective treatment. These can involve walking, exercising, journaling, sports or seeking out friends when the urge to cut is present. Taking care to remove objects that could be used to cut or harm is another option. The rubber band and card with a loved one's name were both very good choices, but sometimes several rubber bands to snap and several deterrent cards may be needed if the urge to cut is strong. Some people have had success in substituting less harmful means of injury for more dangerous ones, such as carrying or having nearby a theatrical knife with a collapsing blade rather than a real one when the urge to cut arises.
Hardly anyone wants to be hospitalized, especially for psychiatric reasons, but this is sometimes the only way to stop repeated and serious attempts at harm. Cognitive therapy to identify and correct the feelings and thought patterns that may trigger self-harm can be done in an outpatient setting, as sometimes can biofeedback, through which people can learn to sense the mood or feeling state that gives rise to self-harm as it is developing and do something about it at an early stage. Medication treatment usually does not involve the most powerful psychiatric drugs, but rather newer antidepressants that ate also effective for anxiety. Natural options for managing depression and anxiety can be taken on your own, although supervision by a physician is a good idea, and include herbs like chamomile, lavender, valerian, St. John's wort and skullcap, supplements like calcium, magnesium and the calming chemical transmitters GABA and 5-HTP and anxiety-relieving homeopathic remedies like ignatia, pulsatilla or sepia.
March 1 is Self-Injury Awareness Day around the world, and many people who are aware and sympathetic, or who have been there themselves, wear orange wristbands or ribbons.
- Photo courtesy of SteadyHealth