Seeing blood in your stool can be very disturbing. It may appear on toilet paper when you wipe yourself after a bowel movement, and in certain cases, it may accompany the stool. Blood in the feces indicates bleeding somewhere in the digestive tract, and even though this seems to be very serious, this is not always the case.
Explained below are some of the more common causes of why you may be seeing or pooping blood along with your feces.

Anal Fissure
Anal fissures usually occur after long-term constipation, when large or hard stools are excreted because of strained bowel movements. There is often pain and bleeding during defecation, and muscular spasms of the anal sphincter (contractile ring at the end of the anus) are also experienced in some cases.
Causes of anal fissures include chronic diarrhea or constipation, inflammatory bowel diseases, and in rare cases, anal cancer, syphilis, herpes or tuberculosis.
The most common symptoms are pain (mild or severe), bright red blood in stools or toilet paper, and itching around the anus.
Anal fissures usually heal after certain dietary and lifestyle modifications. Extreme care needs to be taken for the defecation process to remain as easy and comfortable as possible. However, if the fissure increases in size and symptoms become severe, surgical treatments are available as well.
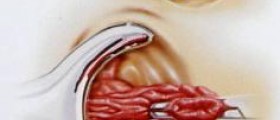
Hemorrhoids
Hemorrhoids, or piles, occur when the veins of the anus and lower rectum become enlarged and inflamed due to pressure. Hemorrhoids can be internal (occurring inside the rectum) or external (occurring under the skin surrounding the anus).
Hemorrhoids can occur due to many reasons, such as chronic diarrhea or constipation due to an unhealthy diet, obesity, anal intercourse, prolonged sitting positions, and strained bowel movements. The veins around the anus and rectum can also bulge and swell due to pressures exerted during pregnancy.
Signs and symptoms of hemorrhoids include painless bleeding during defecation, itching of or around the anal region, swelling of the anus and fecal incontinence.
Many effective treatment options are available for treating hemorrhoids. Most often, dietary modifications and home remedies provide relief; surgery to remove the hemorrhoids is needed if they become very large or problematic.
Chronic Constipation
It is difficult to define constipation, since the frequency of stools varies for each individual. However, chronic constipation is generally defined as having a bowel movement less than three times a week, for several months.
The underlying cause of constipation is usually related to disorders in bowel function. Common causes include an unbalanced diet, inadequate exercise, resisting or disrupting normal bowel movements and over-use of laxatives or antacids. Psychological factors such as stress, depression and eating disorders can also cause constipation. Hormonal disturbances (hypothyroidism) and neurological diseases (Parkinson's, multiple sclerosis) can also lead to constipation.
Symptoms of chronic constipation are straining while passing feces, feelings of incomplete relief after defecating, abdominal discomfort, and swelling. Occasional diarrhea can also occur because of compacted stools blocking the colon.
Treatment includes medication, such as laxatives, and dietary changes, mainly a high-fiber diet and drinking adequate amounts of water.
Some rare causes of why you might see blood in your feces include:
- IBD (inflammatory bowel diseases - ulcerative colitis, Crohn's disease)
- Diverticulosis
- Proctitis
Although bleeding while defecation is not always dangerous, it is important to visit your doctor if the symptoms persist for more than 24 hours. Per-rectal bleeding can be a sign of fatal disease.
In elderly patients, painless rectal bleeding is a hallmark feature of colorectal carcinoma.