Human Papillomavirus, or better known as an HPV infection, is a complicated illness that all patients should be well-educated about. The reason that there is much confusion about this disease is that of the fact that there are some subtypes of this disease. Some of these strains are problematic but not life-threatening while more advanced forms of are something that patients need to be aware of because it could kill them. Here, I will cover some of the more common subtypes and what you can do to help protect yourself from this virus.
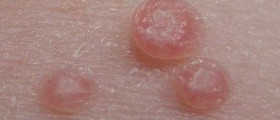
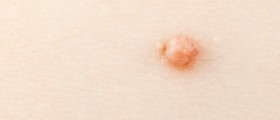
HPV is considered to be one of the most frequent sexually transmitted diseases in the world, and some of the most potent low-risk strains are referred to as HPV 6 and 11. Don't be fooled by the term "low-risk" here, these type subtypes of HPV are responsible for nearly 90 percent of genital warts that patients with an active HPV infection can suffer from. These are outgrowths of tissue usually located around the vagina but can become painful if left untreated. It is also possible for patients who frequently practice oral sex to have these lesions appear around the corners of their mouth.

Thankfully, there are treatment options to remove these blemishes and patients can benefit from a combination of topical antibiotics, cryotherapy, and surgical excisions to remove genital warts. They can be easily prevented through the routine use of condoms to prevent the transmission of this strain of STD.
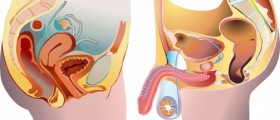
Some of the more serious HPV strains that you must familiarize yourself with include HPV 16, HPV 18, HPV 31, HPV 33, HPV 45, HPV 52 and HPV 58. In reality, the first four are the ones that are most common, and they will be the ones that I focus on here. These types of HPV infections are more problematic because of the high likelihood that these HPV infections can transform into cervical cancer. Cervical cancer is fatal cancer and is highly aggressive so patients who become infected and who do not go to their gynecologist before noticing bloody vaginal discharge will typically have poor prognoses.
Patients can reduce their chance of these strains of high-risk HPV through condom use and undergo frequent speculum examinations to make sure that any irregular histologies are caught and managed before they transform to cervical cancer. These tissues can be removed through surgical interventions in most cases.
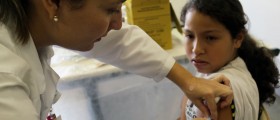
The best way to treat this condition is never to have to deal with it in the first place. Abstinence may be one way to achieve this but this is not a realistic approach in the general population. Advancements in science have lead to the discovery of a vaccination against HPV 6, HPV 11, HPV 16 and HPV 18. This type of vaccination should be given to any girl between the ages of 9 to 26 and will provide immunity against not only the possibility of genital warts but also protect against potent cervical cancer. In most countries, this is a routine shot given to girls between 11 and 12 years old. If you fall into this category, get a vaccination as soon as possible. [1]
You are still at risk to high-risk strains like HPV 33 and 35 and studies show that vaccinations in women older than 26 are less effective so exercise proper preventative measures to ensure you are protected.
- 1.) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2492590/
- Photo courtesy of SteadyHealth





_f_280x120.jpg)